Alina Habba told the court this morning that Trump doesn’t want to testify before the NH primary, and her parents have covid & she wasn’t feeling well. The judge granted a continuance until tomorrow, then Trump posted 44 attacks on Carroll in 20 minutes. https://t.co/ansi9gg97x
— Ron Filipkowski (@RonFilipkowski) January 22, 2024
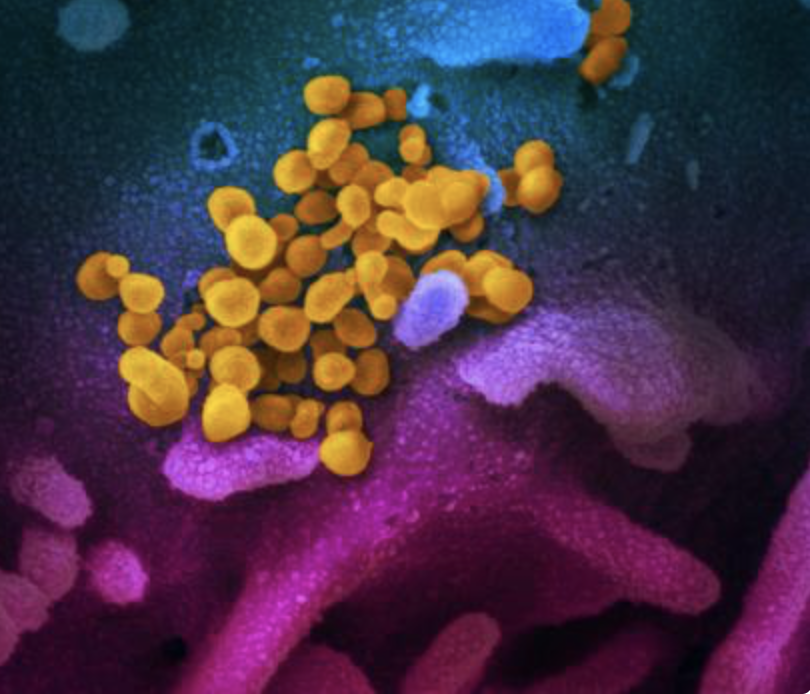
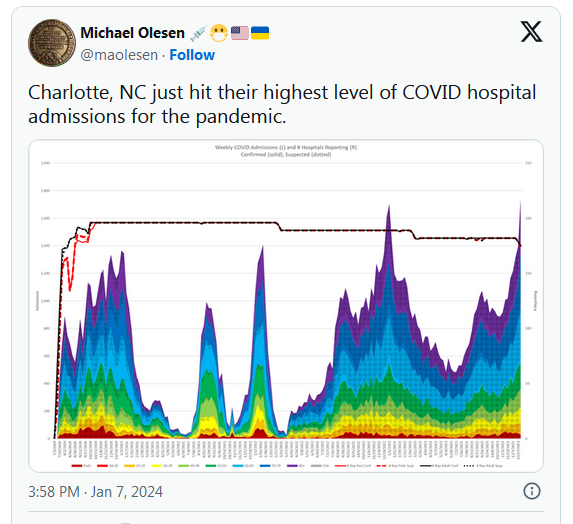
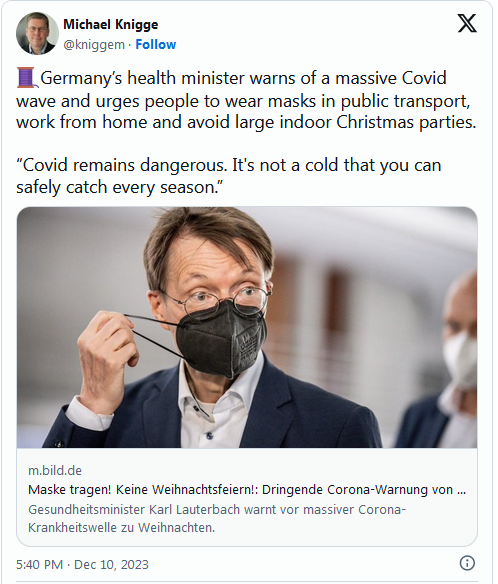
Rhinovirus (Covid / flu / RSV) infection exposure is certainly a possibility right now, but nothing in our corrupt reality can be separated from POLITICS…
What actually happened:
Trump’s lead attorney Alina Habba asked for an adjournment after she and a juror may have been exposed to COVID — and the judge granted that request, over the objections of E. Jean Carroll’s lawyer. https://t.co/tAdNDyLa9e pic.twitter.com/0BN3HPWV9D
— Adam Klasfeld (@KlasfeldReports) January 22, 2024
Monday Evening Open Thread: The Covid Ate My Legal BriefPost + Comments (92)