Earlier this year, the Supreme Court ruled that insurers were still owed about $12 billion dollars in risk corridor (RC) payments from the 2014-2016 policy years from the fully insured small group and newly regulated individual health insurance markets. Risk corridors had the federal government promise to take on some of the losses of insurers that systematically mispriced the market in 2014-2016. Insurers would be able to collect these sums through the normal federal judgement paying funds. Those funds take a little while to process, but the wheels of payment started over the summer.
One of the wonkier questions was how would the Center for Medicare and Medicaid Services (CMS) treat these RC receivables and how Medical Loss Ratio (MLR) calculations would be made.
Last night, CMS released their initial draft guidance.
It is fascinating (to me, a few dozen wonks and every ACA participating insurance company CFO).
TLDR: MORE HOOKERS AND BETTER BLOW
MLR regulations for the ACA are straightforward in concept if somewhat confusing in execution. Over a three year period, the qualified claims and quality improvement expenses have to be at least 80% of the qualified premiums collected. If the individual market insurer has an ACA MLR above 80% nothing happens. If the ACA MLR in the individual market is below 80%, the insurer owes the policy holders in the last year a rebate to true up the 80% calculation. These rebates are distributed on the basis of the proportion of gross premiums a policy holder has relative to the entire pool of rebate eligible policy holders. Weird things can and do happen. Negative net premiums are quite plausible.
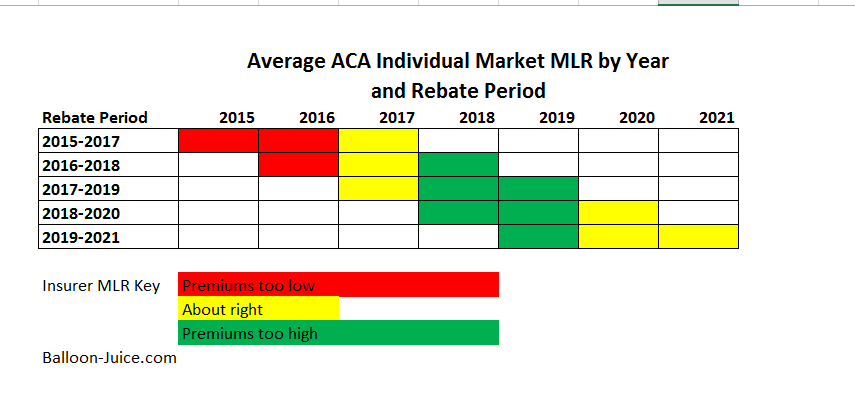 Insurers in the individual market paid out tiny MLR rebates in 2014-2016 cycle nor much more action in the 2015-2017 cycle. Modest MLR rebates were paid for the 2016-2018 cycle as 2016 was still systemically underpriced, 2017 was appropriately priced, and 2018 was grossly overpriced due to silverloading. 2019 was overpriced and 2020 looks to be overpriced as well. 2017-2019 rebates are significant. 2018-2020 rebates are likely to be even larger.
Insurers in the individual market paid out tiny MLR rebates in 2014-2016 cycle nor much more action in the 2015-2017 cycle. Modest MLR rebates were paid for the 2016-2018 cycle as 2016 was still systemically underpriced, 2017 was appropriately priced, and 2018 was grossly overpriced due to silverloading. 2019 was overpriced and 2020 looks to be overpriced as well. 2017-2019 rebates are significant. 2018-2020 rebates are likely to be even larger.
Under previous rules, a receivable would be applied to the current year MLR premium denominator. A big cash infusion would mean, all else being equal, the proportion of premium dollars spent on qualified claims and quality improvement efforts would be low to very low. Pragmatically it would make 2020 look to be extraordinarily overpriced with massive rebates.
There are notable distributional problems with this. People who paid too much in premiums in 2014-2015-2016 are getting screwed and the people who buy 2020 plans are getting a massive windfall as most of the Risk Corridor cash settlement would distribute out to current policy holders as insurers were already close if not already under the rebate line for the 2018-2020 period. A huge cash infusion would pump up the denominator and push a lot more insurers into a rebate position.
Another other option CMS could adopt was to say that risk corridor funds should be accrued to the years that they were supposed to be paid and then have MLR recalculated for those years.
This is the track that CMS proposes to do. It is a logical pathway. The risk corridor obligations were generated in 2014-2016, so when they finally arrive into the insurers’ vaults, they should be credited to those years. This is straightforward accounting. MLR calculations will be run and any payments that are now owed will be paid.
This makes sense.
It is also a decision that is a huge windfall to many insurers that will enable the age old question of “More hookers or better blow” to be settled with a simple answer: “BOTH!”
We know that insurers lost massive amounts of money from 2014-2016 on the ACA individual market. Raw MLRs were in the high 90s and at times well over 100 where claims were greater than premium revenue. There were a few profitable insurers that kicked in miniscule MLR rebates. But there were not many insurers that lost enough money to be RC receivable AND also had ACA MLRs just above the refund line. A big cash infusion for those few insurers will generate MLR rebates that will eventually go into consumers’ hands. However, the more likely scenario for insurers that are now receiving RC funds after the favorable Supreme Court ruling will be that they lost a massive amount of money in 2014-2016 which generated the RC receivable and in the process of losing a massive amount of money, their MLRs were wicked high. So once the RC money lands and accrues to the correct years, the re-estimated MLRs are still above the refund limits. At that point, the RC money is free cash flow to the insurer.

Another Scott
Interesting. Thanks.
I hope our good friends at the IRS are carefully looking into how the insurance companies handle this stuff. Presumably (though IANA tax lawyer) the insurance companies could claim large losses in the bad years and presumably would have to file amended returns if they were to soon get a windfall to cover those losses (and more). I’m also sure that stuff like this happens all the time when expenses are now but extra income is later. But we need unbiased observers checking to see that the insurance companies aren’t playing “heads I win, tails you lose” with their tax obligations.
Cheers,
Scott.
Frank McCormick
I am currently awaiting a $1300+ rebate check from BCBS of TX as their MLR was only 70.5% for the individual market for 2019!
Ken
I asked this in the previous thread, but since this is David’s maybe it’s better here. The Senate Republicans are staging some kabuki where they vote on a bill guaranteeing coverage of pre-existing conditions, in case the court overturns the ACA.
Now I have a vague memory from David’s posts, and a vaguer one from the original analysis for the ACA, that requiring insurance companies to cover everything but not requiring people to buy insurance is a Bad Thing, both for the companies and for consumers. Is that the case?
(Not that I expect any analysis has been done by the Republicans, other than “Jesus over 60% of the public likes the ACA that we’ve been running against for over a decade and now the court is going to strike it down whadda we do whadda we do.”)
randy khan
I have some vague, and possibly incorrect, recollection that the idea behind the risk corridors was to insure (sorry, but not really sorry) insurers against exactly what happened in the early years, in which case the decision to apply the money to those years actually is correct.
Or, put differently, the hookers and blow budgets got nailed in those years, so now they will be returned to normal levels.
David Anderson
@Ken: Will answer tomorrow morning!
Ken
@David Anderson: Tease!