Georgia has prepared a complex 1332 waiver for their individual market. It has two parts.
The first part is a reinsurance waiver that varies the pay-out by county and degree of rurality. The objective is to bring down premiums for unsubsidized buyers. This part of the waiver would go into effect for January 1, 2021.
The other part of the waiver is an attempt to operationalize Ted Cruz’s amendment during Repeal and Replace.
Here is how Vox described the Cruz Amendment:
If an insurance company offers at least one plan in the state that is compliant with the (Obamacare) mandates, that company can also sell any additional plan that consumers desire.
What that does is it maintains the existing protections, but it gives consumers additional new options above and beyond of what they can purchase today….
That is true. But outside experts argued that the costs to the federal government could be unsustainable. As the Obamacare markets turned into high-risk pools, premiums would increase, driving the cost of the tax subsidies higher and higher.
“Keeping the ACA tax credits would, in theory, protect subsidized consumers,” Larry Levitt, senior vice president at the Kaiser Family Foundation, told me. “But the cost of those tax credits would quickly skyrocket, because healthy people would flock to non-complaint plans, which could cherry pick them with inexpensive premiums.”
Cruz acknowledged that his plan would depend on taxpayer subsidization of people with high medical costs. But, he argued, it was better for the federal government to pick up the tab than requiring health plans to charge sick people and healthy people the same premiums, increasing costs for the latter.
The second stage of the Georgia 1332 proposal would do a few things.
- Redirect all federal subsidy money to a Georgia state government account
- Maintain full Essential Health Benefit plans that set subsidies levels
- Allow insurers to offer subsidy eligible plans that don’t offer all 10 Essential Health Benefits
- Inject state funding to pay for extra subsidies for the new enrollees
The critical thing from a legal standpoint is the last point: the state is bringing in a lot of new money so that the seriously ill won’t be worse off if they purchase the benchmark silver plan which will be more than sufficient to meet guardrails.
The concept of operations is that insurers will offer a limited portfolio of full benefit plans and a bunch of much cheaper limited benefit plans.
ACA plans are required to offer 10 Essential Health Benefits (EHB). Milliman has a good graph that shows where the money is spent on EHBs:
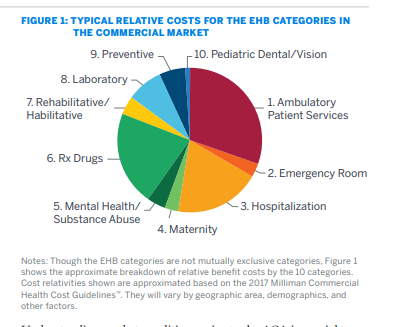
For instance, Mayhew Insurance could offer a full benefit Silver plan and a limited benefit silver plan that covers everything except maternity, labor and delivery. The limited benefit plan will have about a 3-5% cost savings compared to the full benefit plan in a static analysis. However, the cheaper, limited benefit plan will actively repel any woman between the ages of 15 to 40 who thinks that there is the vaguest chance in hell that they will be pregnant. All of the pregnancy risk will be concentrated in the full benefit plan. The premium spread between the full benefit plan and the limited benefit plan will be greater than the total cost of the service as the risk will be concentrated in the full benefit plans.
I could easily see most insurers offer limited benefit plans that exclude maternity, pediatric dental/vision, and most of the preventive care benefits whose pay-out period is more than a year. More complex plans would have those exclusions plus limits on prescription drugs such as not paying for hepatitis-C drugs which is worth several dollars per member per month in premiums. Anyone who had any reasonable risk of needing the excluded services will go to the full benefit plans.
This is a way to convert the ACA individual market into a fairly well funded high cost/high risk pool. The low cost/low risk will self-underwrite to the subsidized limited benefit plans while the sick will overwhelmingly select the full benefit plans that have the same subsidy schedule for 100% to 400% FPL. The sick or high risk to be sick and expensive who earn over 400% FPL will truly be SOL under this scheme.
There are several major operational challenges. The first is how are the limited benefit and full benefit plans linked. Are they linked via risk adjustment where the limited benefit plans send significant chunks of premiums to the full benefit plans? That would lower the gross premiums for the sick and earning over 400% FPL while increasing state subsidy spending and costs for the healthy. Would reinsurance be assumed to be doing enough work here to keep the sick 400% FPLers close enough to the non-waiver status quo so that the limited benefit plans and the full benefit plans are linked to a common index rate like Catastrophic plans are currently linked to today? Are the limited benefit plans risk adjusted against themselves?
The legal vulnerability is that the state of Georgia is placing a cap on total 1332 spending of about a quarter billion dollars a year for both extra subsidies and reinsurance. Subsidy disbursement will be capped. If there is significant take-up of plans, people will be signing up late and not receiving assistance. Furthermore, if the morbidity profiles are worse than the state assumes, there will be obligations that are just being abandoned.
I’ve long thought that a variant of this idea makes a lot of sense. The one major change for a fix it and forget it policy would be to lift the subsidy cap from 400% FPL. California has done this to a limited degree to 600% FPL but opening up the subsidy schedule so that no one pays more than 10% of their income for a benchmark plan would get rid of the problem of a family of four paying $30,000 or $40,000 for coverage if they are old enough.


 On The Road – Mike in Oly – Tucannon River, WA
On The Road – Mike in Oly – Tucannon River, WA
Searcher
Technically I agree with Cruz, because the federal tax dollars come from progressive taxation and healthcare premiums represent a flat tax, but assuming it’s the Cruz I think it is I assume it is just a trick to make the ACA look like a failed, expensive program.
rikyrah
Sorry don’t trust it. After all, this is a state that still refuses to do Medicaid expansion ?
JPL
@rikyrah: I tend to agree and I live here.
Mormo
@rikyrah: Indeed. How isn’t this just yet another iteration of privatize profits, socialize costs? With an additional “benefit” of yet more complexity that can publish people who didn’t realize they signed up for the a Screw You plan?
At this point several states have demonstrated successful ways of “innovating” within the obamacare framework without Fucking The Poor and maybe we should be using those states as lab models for increased coverage and stable, competitive insurance markets. Like California! Outlawing Screw You plans works! Expanding Medicaid works! California has maternal mortality rates like Finland!
DAVID ANDERSON
@Mormo: can you get a working majority for your favored policies in Georgia. That is a binding constraint.
ThresherK
Wait, Ted Cruz? I really didn’t read this post. I just got back from scraping the snow off my wife’s car. I haven’t brushed my teeth or had my breakfast or caffeine.
But my autonomic nervous system is telling me anything with his name on it is a bad idea.
Joe Falco
Georgia Republicans would put up a constitutional amendment to forever outlaw the ability of the state government to adopt an unvarnished Medicaid expansion if they thought it would pass with voters. There’s no telling what depths they would sink to in order to deny a victory to Obama and Democrats.
Mnemosyne
As always, I have to shake my head at the people who are 100 percent convinced that neither they nor any of their covered family members will ever get into an accident or get sick unexpectedly, so they decide they don’t “need” health insurance. ?
LongHairedWeirdo
I confess, it never ceases to amaze me how the GOP gets away with saying “it’s better for the government to make welfare payments, than for insurance to be insurance.”
Mormo
@DAVID ANDERSON: Yes, absolutely in the politically accomplishable sense! And there isn’t such a majority. I honestly love the level of attention & thoughtfulness you bring, but in myself I recognize the temptation to attend to complex solutions because it’s tempting to me to think about, not because it’s a better solution. Let’s spend attention on what seems to be working and isn’t in states that are actually trying, especially since many of us here suspect state Republicans of acting increasingly rationally, to secure federal money and under voter/lobbyist pressure to support rural hospitals.
My only quibble, and it’s small, is the degree of respect with which you seem to engage with Republican ideas/plans. My assumption is that in this area state Republicans have mostly started acting in bad faith, like complicating voter approved Medicaid expansions, because their actual ideas (Fuck The Poor) are so overtly unpopular. Really appreciate all your writing.
ccswood
So sorry, I meant to comment here. Can you delete the one on the Nov 5 post?
There were five public hearings to present both this waiver and the one dealing with Medicaid. It seems to me that the locations chosen were not logical if the intent was truly to solicit the most public involvement. There was one in both Macon and in Savannah. However, three others were in Rome, Gainesville and Kennesaw, all small towns north of Atlanta, two of which are in the blue reinsurance regions on your map. The last was in Bainbridge (also blue on your map), population 13,000, which is located in the most extreme SW county in the state. That location, while an hour away, was the closest to me in Albany, the major city of SW GA with a metro area population of 157,000 and a seemingly better place to hold the meeting. There were no hearings at all in Columbus, Athens, Augusta or Atlanta.
I did not attend the “closest” meeting but I ran across this article which goes over the 1332 waiver request in pretty good detail.
https://www.healthaffairs.org/do/10.1377/hblog20191105.878300/full/
Kemp proposes to eliminate access to the Federal ACA website and will direct everyone to multiple profit minded websites run by brokers and insurance companies. Websites will offer both ACA compliant and non-compliant plans, hopefully clearly marked and quality rated.
“Georgia believes that this decentralization of enrollment (i.e., a shift away from a single platform like HealthCare.gov to multiple enrollment channels) would promote competition, improve customer service, and drive enrollment.” Because this certainly seems easier than the “poorly run” HC.gov site!!
Subsidies will be state specific and may not match the feds after the first year. Georgia’s contribution to these funds will be subject to the whims of the legislature. A good portion of Georgia’s contribution will also have to go towards back end administrative functions now performed by the feds.
“The state could amend this subsidy structure in the future based on actuarial analysis, funding levels, and enrollment.”
“However, Georgia would cap its contribution towards the Section 1332 waiver on an annual basis. Unlike in the current individual market, this cap could result in waiting lists even for individuals who qualify for subsidies. Georgia notes that subsidies will be granted on a first-come, first-served basis until the state’s funding cap is reached. If there are a larger number of subsidy-eligible residents than expected, those individuals could still enroll in coverage but would be placed on a waiting list for subsidies (meaning they would pay full premiums even though their income would qualify them for subsidies under the ACA).”
So, just because you qualify for a subsidy does not mean that you will actually get one? Each Nov 01, all of us are supposed to duke it out for the available funds? How much time will they take to notify you as to whether you qualify? Guess that you might have to be prepared to quickly cough up another $1000 per month (if you are old and poor) or move out of state?
Hunger Games and medical emigration?? Disrupt 450,000 in order to add only 30,000 additional insured? And they call this the Patients First Act?