Yesterday, the Center for Medicare and Medicaid Services (CMS) released a guidance letter to state Medicaid directors saying that CMS would welcome Section 1115 Waiver applications that contained work requirements. The guidance would not provide any extra money for supportive employment or services and it’s logic chain of justifying employment as a condition of receiving healthcare continually confuses correlation and causation. It is a guarantee that there will be a lot of lawyers involved once the first 1115 waiver with work requirements is approved.
Kentucky is highly likely to be the test case. Their 1332 waiver is heavy on work requirements and it is likely to be approved within the next week. Functionally it is designed to force adults off of Medicaid by either explicitly disqualifying people for not working or volunteering enough or by creating paperwork hassle barriers. At the end of the fifth demonstration year, Kentucky projects that roughly 90,000 fewer adults will be covered by Medicaid.
There is something odd in the budget justification. The Per Member Per Year (PMPY) costs of the adult population is projected to be strange for the Legacy Medicaid adult population.
For a guaranteed issued, low or no premium plan, one usually expects that the people with the most significant needs are more likely to sign up and jump through eligibility hoops than people with low expected medical needs. The first person to sign up is far more likely to have cancer or cystic fibrosis or hemophilia or anything else that can routinely create a $100,000 claim than the last person to sign up. We should expect the PMPY to decrease as enrollment goes up and vice versa. The marginal/incremental covered lives are more likely to be healthier/cheaper than the average covered life.
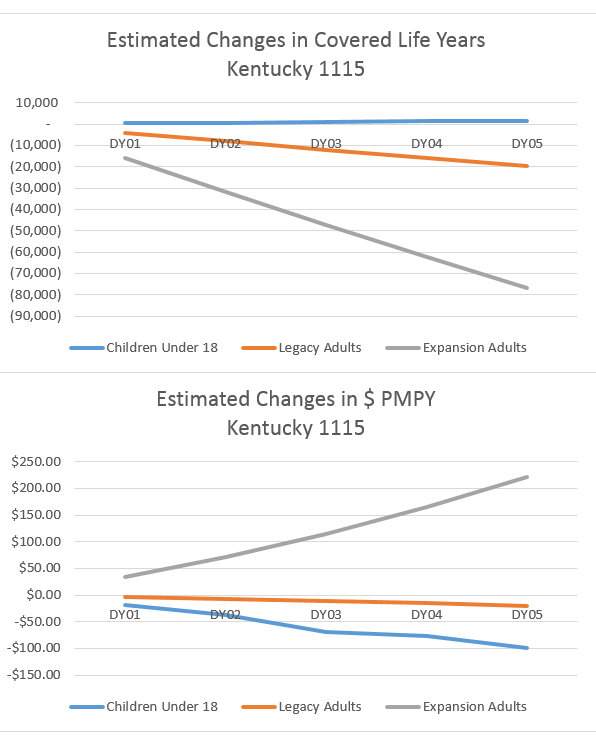
We see that relationship in the Adult Expansion population. By the end of the demonstration, the Adult Expansion population is 15% smaller but the PMPY is 2.4% more. I am unable to look at either the actual claims or the actuarial model that projected the drop-off but the direction makes operational sense. We see the same with the kids as there are slightly more (0.3%) kids covered with a 2.6% reduction in PMPY. The gearing ratios are very different but they are both going in the same direction.
However the Adult Legacy Medicaid covered population which is overwhelmingly medical condition based (including pregnant women) is projected to decrease by 14.1% while costs on PMPY basis decrease by 0.2%. This is odd where enrollment and costs are going in the same direction. The Legacy Adult group has significant variance in medical status so one would expect the individuals with the worst health are more likely to stay than people who either qualify on the basis of income but are in otherwise “decent” health or people who barely qualify on the basis of health status.
This is strange. There might be a good actuarial reason but it is strange on first glance.

Mnemosyne
Honestly, I fully expect that the 14 percent reduction for Adult Legacy comes from thowing disabled people who can’t work off the rolls. I’m definitely glad that my friend’s severely epileptic sister has moved back to California where she can get the healthcare she needs since people
Ike her with “invisible” disabilities are probably going to get screwed first.
Timurid
PMPY ain’t easy…
schrodingers_cat
I hate these twenty first century Mir Jaffars like Seema Verma and Nikki Haley.
dr. bloor
Arbeit Macht Gesund.
Timurid
@schrodingers_cat:
And Raj Shah and Ajit Pai…
Fuck those guys.
Victor Matheson
Does this mean that Kentucky can now officially be classified as a “shithole”?
Probably too many white people to qualify, I would guess.
schrodingers_cat
@Timurid: I know some Pais, wondering if they are related to this asshole. Its a fairly common north Karnataka last name, so may be not.
eclare
@dr. bloor: Clever, I like it.
TriassicSands
@Mnemosyne:
Clearly, your friend did the right thing by moving to a state that is hellbent on punishing poor people. Of course, the more people that do that the redder the barbaric states get and the further they are from being civilized. In time, we could end up with a permanent Republican minority nationally that always controls the Senate.
I just heard Jeff Colyer, the Republican lieutenant governor from Kansas, explaining why the work requirements are really good for the people on Medicaid. He’s making it sound like it’s going to be easy to get an exemption. Hey, I’m convinced!
Rumor has it that Kansas, after massive economic mismanagement, needs to save money. And we all know where the money is — the poor.
TriassicSands
@dr. bloor:
Und frei.
Which is what Kansas Republicans probably want to poor to work for. If only they could abolish the minimum wage.
Russ
So is this article misleading in that a work requirement would be illegal?
http://familiesusa.org/blog/2018/01/six-reasons-work-requirements-are-bad-idea-medicaid
TriassicSands
@Victor Matheson:
Kentucky? I think it is fair to say the whole country can be classified as a shithole. I live in a reasonably blue state — Washington — and don’t consider it to be a shithole, but the reality is that outside our borders we’re one country led by one disgusting idiot who is turning this country into a real shithole.
So far, from what I’ve been able to glean, people in other countries, while appalled by Trump, have been quite forgiving of those of us who didn’t contribute to this mess. Many seem to express sympathy for us. That may continue until Trump feels he has to start a war to divert attention from all his “winning.”
David Anderson
@Russ: I think there is a good argument that work requirements contravene the objectives of the Medicaid program and thus are not waive-able.
However I am not a lawyer, I am especially not an administrative/health law lawyer.
There will be billable hours!
Brachiator
I am not even sure what they are trying to correlate to justify employment as a condition of receiving health care. Maybe I could see some incentive to get private health insurance, but even that’s a stretch.
Yutsano
@David Anderson:
That has to be part of the epitaph of this mis-administration.
Mnemosyne
@TriassicSands:
Um, I think you misread my comment, unless Jerry Brown is up to shenanigans we haven’t heard about.
TriassicSands
@Mnemosyne:
My problem. “To” should be “from.” Sorry.
Your friend did the right thing moving from a state…
Mnemosyne
@TriassicSands:
Well, I’m not going to lecture disabled people about how they should stay in a shithole state where their healthcare is getting cut off so they can suffer for the rest of us. Let able-bodied people move to Mississippi if they’re so goddamned concerned.
Lee
To utilize a current meme:
The leopards in Kentucky are are going to get very fat from all the face eating.
But her emails!!!
@Lee:
True, but they aren’t going to have insurance to cover all there obesity related health ailments, so there’s that.
Aardvark Cheeselog
I’d go with “wishful thinking.”
SteveNKY
It appears the waiver was granted. What will the black-lung coal miners do now? Stand at the crossroads of their deserted two street towns with tin cups in their hands?
Hard lessons are the only lessons learned for a lifetime.
May all KY learn from the votes they cast or didn’t cast.
Matt
@SteveNKY: They’ve been voting for people who gleefully fuck them over (just as as long as they say “PRAISE JEEBUS” while doing so) for decades now, I don’t see much chance of learning.