I like Kevin Drum but he is getting this wrong:
It’s true that Obamacare enrollees tended to be sicker than pre-Obamacareindividual enrollees. But that’s not because Obamacare enrollees are especially sick. In fact, they’re nearly identical to people enrolled through employer plans, which take all comers and therefore come pretty close to representing the average patient in America….
the BCBS report concludes that Obamacare enrollees used more medical services and ran up higher bills compared to those in employer plans. That’s a little hard to make sense of, since Obamacare enrollees are no sicker than average andgenerally have higher deductibles and copays than people in employer plans, which should motivate them to use fewer medical services.
Here is the actual Blue Cross and Blue Shield methodology:
The data in this report include approximately 4.7 million individual members and approximately 25 million employer-based group members and focuses on members ages 21 through 64. The impact of the federal risk adjustment program for the individual market is not reflected in this report. The charts report statistics calculated with the first nine months of claims data for each year because the medical claims for the fourth quarter of 2015 were not available at the time of publication. Using only the first nine months of data for both years ensures comparability. Data on medical spending are reported in terms of “allowed” medical costs [my emphasis]
The first problem with Kevin’s analysis is that BCBS dealt with the cost sharing problem by looking at the maximum contract rate for the service before any member cost sharing was applied. Secondly, Andrew Sprung at Xpostfactoid is pointing out that ACA Exchange policies look a lot like ESI policies in terms of cost sharing:
The average AV for a HealthCare.gov enrollee is just a point below that of a gold plan (80% AV). And this estimate may be conservative, since, again, CSR takeup is higher at lower income levels. Only 17% of silver plan buyers on the federal exchange ended up with the 70% AV often cited without qualification as the value for silver.
Average employer sponsored insurance (ESI) has about 80% actuarial coverage. There is minimal difference in terms of average cost sharing and induced demand.
More importantly, the differences that Kevin is poo-pooing as minor and insignificant are very significant:
@bjdickmayhew And also would argue that it’s still wise to wait a few years. Diffs of a few percent have a habit of changing considerably.
— Kevin Drum (@kdrum) March 30, 2016
Here is the percentage differences of utilization and disease categories in the report:
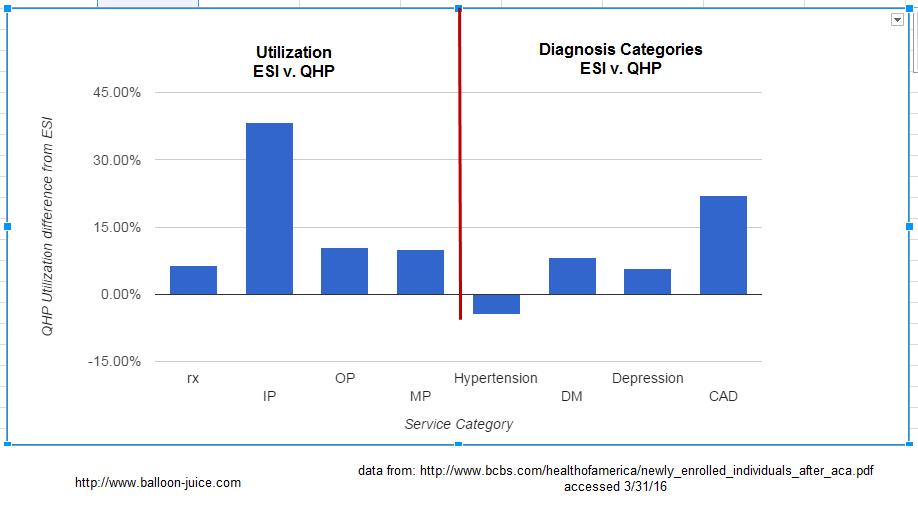
Speaking as an insurance professional who can’t run stats on my smart phone while I am on the bus this morning, an eyeball test is telling me that over millions of covered lives, differences of 10% of utilization for outpatient and medical professional claims is operationally significant. Inpatient (the most expensive part of the entire medical system) is up almost 40% for the Qualified Health Plan (QHP) individual market cohort compared to the ESI group. Speaking as someone who does this for a living, we celebrate as a major success when an initiative drives down inpatient spend and utilization by 2%. 40% differential is massive.
The people who are new to the individual market are sicker and higher utilizers on average than people who get coverage through an employer group. This makes sense for two reasons. The first is that linking insurance to employment and usually full time or near full time employment is a screen for health. If someone is sick with diabetes, depression and coronary artery disease, they are less likely to be working 30 hours per week than an healthy individual of the same age who lives next door to them. Secondly, the people who were new to the individual market and not in the group market were more likely to have not been insured in the months leading up to their enrollment in the individual market. We know that gaps in care lead to higher net expenses for people with chronic conditions. So the story makes sense to me.
I agree with Kevin that this study is showing that the ACA is doing what it should be doing; getting people who need medical care access to medical care. But dismissing clear evidence that there is a significant initial difference in population health is lazy and wrong.

Technocrat
This is one of those subtle things that aren’t obvious until you think about it. At least it wasn’t obvious to me.
This is great stuff, Richard. I hope Kevin reads your posts ;=)
HinTN
Lazy and wrong, touchstones of the commentariat.
Eric S.
Is the key “initial difference? ” Do you expect over the course of some years the two populations will begin to have similar usage patterns?
I know I’m in that 40% group. I was playing Russian Roulette for a while then bought in. I want sick but sustained two sports injuries, one requiring surgery.
Dupe1970
Nerd smack down! Although I do like Kevin Drum and his reporting on lead poisoning especially from vehicles and crime rates was very excellent.
Cermet
ACA is working EXACTLY as it should! Helping many in need who previously couldn’t dare get help due to costs/pre-existing condition issues. Thank you President Obama – your the man! Exactly what a Dad does for his children – looks out for all of them; even the ones who voted against him (I’m looking at you Appalachia residents.)
MomSense
Trying to educate us jackals isn’t challenging enough for ya Richard? Now you are going to try and work with the punditubbies?
This should be good.
Richard Mayhew
@Eric S.: My personal belief with no real evidence is that the individual market will always be a little sicker on average than the ESI market because the individual market is a “use it until something better” universe. ESI is usually something better.
I think the differences will shrink over time as catch-up care starts to subside (we are seeing that already) BUT I think the difference will still be there in 10 years.
Jeffro
OT until we get an open thread but you have to love the transparency here:
http://talkingpointsmemo.com/livewire/greg-gutfeld-internal-strife-fox
Actual quote from Gutfeld:
“On any given day, we have tension over this nomination, over this candidate. You can look at our network as a whole, which is — don’t look at me — but you can look at this network, where we are having issues within a family of anchors over this stuff. You can look at the Party,” Gutfeld continued. “So at every area where there is conservatism, there is strife.”
The Fox host then fondly recalled “the good old days where we could all unite against the hatred for Obama, when it was so easy.”
And that really is the modern GOP in a nutshell: remember the good old days, when Obama-hatred was enough to get us through the trying times?
Sigh…
He goes on:
“…but somehow, Trump has shattered that, and now we’re sitting here, we’re grappling with this internal strife and we have no way to get out of this.”
Sure you do! Start a new party based upon some actual conservative principles, even if they are misguided and selfish, Greg!!
Brinks Truck Driver
My vague impression was that the Blues tended to have the broader networks on the exchange, which made them especially appealing to sicker individuals (on the exchange). Is that true, and Is there any way to tell how much that might be driving the difference here?
Richard Mayhew
@Brinks Truck Driver: The Blues on the whole tended to have fairly broad networks at least in 2014. Big changes in 2015. This is not a completely random sample, but it is probably 25% of the individual market covered lives and a very reasonable chunk of the entire ESI covered life universe so even if not 100% generalizable, it is an extremely valuable window into a big chunk of the covered population.
rp
“bjdickmayhew”?
japa21
There are obvious differences here that Kevin minimizes, which is actually a journalistic blunder. But I think the real problem is that very few people, including many in it, really understand health insurance. It is a totally different animal than any other insurance out there.
Richard, you perform a great service helping the BJ community get a better grasp of it.
Fair Economist
Exchange insurance is still expensive enough that many people are deliberately planning to not buy it. I don’t see how purchasers could *not* be sicker on average for employer-based policies, which is a more-or-less random sample of those healthy enough to work. There are two big reasons, disability and self-selection, which will both drive down the relatively healthiness of the Exchange population.
gvg
I knew there was a correlation between not sick and employed. I do financial aid for college. Professional Judgement petitions will have us doing an income reduction due to parent sickness and medical costs one year. the next year it is the same parent is now unemployed. Years ago we had a co worker with terminal cancer who was also in denial about the chances. Our bosses had a meeting with us and very unusually told us that they had researched the rules and Marina could stay on insurance as long as she worked 30 minutes every 2 week pay period so she was going to do that. They also told us that the cancer drugs were affecting her mind at that she was making mistakes, so we would just have to check behind her without her catching on because it would upset her. We would all have to work harder to cover her load, we couldn’t hire someone to take her place etc. In other words it was a real problem to an employer and ours was very unusual it not finding cause to fire her. I don’t care what the laws are, I had already seem a lot of documentary proof that employers found ways to get rid of sick employees because they actually couldn’t do their jobs. Other employees might also resent the work load. There are problems with tying insurance to jobs to say the least.
lowercase steve
I study poverty and labor force participation so Drum’s statement,
immediately made me raise an eyebrow. As you said, the chronically sick (diabetes, depression, etc.) are far less likely to be working fulltime (and thus receiving health insurance through an employer).
gvg
Maybe because of my job, I just had more reason to know with documentation, that you can’t hold a job without at least some health. Many people have just never really thought about it.
WereBear
@gvg: I find it amazing that your employer was so compassionate. I hear lots of stories of people who drag themselves into the office enough to not get fired and hopefully have co-workers who help them keep up with their duties.
It is incredibly cruel to expect someone dealing with a serious illness to also show up at work in order to keep being treated. Most of these people quietly collapse and drop off the radar.
ruemara
@gvg: I lost my job at a magazine after a bp related nose blowout. Thanks hospital, for letting my boss in to see me without asking me so she could see me covered in blood and coughing up blood. I was fired within 2 weeks of return to work.
When they see you get sick, they realize they can’t use you until you drop.
kindness
I like Kevin too. His comments section, not so much. I don’t know though, might be something to do with living in Orange County. Kevin calls himself a moderate/progressive but he far too frequently swallows and regurgitates Republican Talking Points. So I take what Kevin says with boulders of salt.
RepubAnon
@Technocrat: Indeed -it’s one of the reasons insurance companies like employer-based plans: if you get too sick (and thus expensive), you typically either can’t get a job or lose the one you have. Thus, the pool of employed persons is healthier on average – and every healthy person cherry-picked from the overall population makes the remaining members of that pool less healthy on average.
Think of them as the ones last to be picked at a children’s baseball team…
Richard Mayhew
@rp: I needed a Twitter handle that is separate from meat-space me so Balloon Juice Richard Mayhew was too long — that was the first natural abbreviation …
plus I still have the humor of a 15 year old
martian
@WereBear: I know personally of one act of extreme employer generosity. My husband’s old company hired a woman who was shortly thereafter diagnosed with cancer. Insurance had not yet kicked in, there was maybe a 30 day window, and the boss got her on the plan. Being an owner, he could do that, and it was really humane and kind of him. But relying on the kindness of strangers is only a plan if you’re a Republican good ole days fantasist, obviously. Most people won’t luck out like that.
Fred Fnord
Pooh-poohing. Poo-pooing is entirely different.
MomSense
It is possible to work 40+ hours (fully employed) and not have health insurance because your employer is a small business and therefore not obligated to provide health insurance. The problem in the old system was that you earned too much for Medicaid and not enough to afford more than a catastrophic plan and those became too pricey for many of us. Those plans were not cheap in my experience and the deductibles and co-pays discouraged even routine care.
Anyway, many of us fully employed people had spent years either uninsured or under-insured and therefore we were also “sicker” or at least in need of all the diagnostic and wellness things. I wonder if there are studies showing what happens to the employed but not fully insured population. Are/were we more likely to have major health crises and then enter the world of unemployment or unsteady employment?
I would include self-employed people in the employed but not fully insured category.
MomSense
@Richard Mayhew:
Well I think it’s perfect.
amygdala
Yeah, this times a bazillion. There’s a lot of un- and underinsured territory between well enough to work enough hours for an employer with good benefits and sick enough for long enough (without winding up dead) to be eligible for Medicare before age 65.
Richard Mayhew
@Fred Fnord: In my household poo-pooing earns marshmallows for the youngest plus it is a frequent topic of interested and involved conversation.
Mnemosyne
@Jeffro:
This morning, I told G that I’m expecting the RNC to bring Alan Keyes out as the nominee at the convention, because when you need a placeholder so the Democrats don’t run unopposed, Alan Keyes is the guy you call.
Then we laughed until we almost made ourselves sick.
gvg
well I knew it was unusual for the employer to be so humane. I still work at the same place after 20 years. 3 years ago I had cancer and had to use FLMA. I had a number of $20 $40 copays and one $200 surgery copay. No arguments. no problems and my job even allowed me to work when I felt like it. I would have gone crazy at home for months. Its a good way to think to much. Anyway I had a 6 week surgery recovery no work then 6 chemo treatments 3 weeks apart getting weaker each time and taking longer to recover. Felt like getting old and arthritic very suddenly with no stamina. I’d feel ok, then hit some limit and be exhausted with a headache on the spot. so I learned if I pushed, it would take days extra to recover. Basicly it started with 2 or 3 days feeling bad after a treatment then going to work till the next time to taking a week to recover and working 2-4 hrs a day till the next time. then months of getting stronger working longer. They let me do that. I couldn’t even accurately predict if I would be in the next day. I do know that I was appreciated when I got in because they would be backlogged and after I was back a little while, caught up. I had over a thousand hours unused vacation and sick leave when it started. What if I got sick at the beginning of my working life and not after decades at the same place where I had a good reputation? we have no control over that and people mostly change jobs more often.
If they had a history of screwing people, I probably wouldn’t have stuck around. I am a valuable employee. So are a bunch of other long term people. Stuff runs well.
But I have to contrast that with another employee who finally took medical retirement. She never was really reliable about coming in and called in sick alot. her bosses thought she just was using all her sick leave as earned. then she started having multiple serious medical issues. Finally a late diagnoses of Lupus and dr’s didn’t seem to help. She would have been fired pretty soon because of the senior management were frustrated. I can’t tell if she really had always had a poor work ethic (but was very friendly and good with people) or if her health had always been poor. She failed to show up many times where I was one of the people who then had more work. It went on like that for years. Lupus is ultimately fatal and the tests for it are pretty certain.
Mnemosyne
@gvg:
I think most people learn from sad experience that they need to conceal their health status from their employers. I’ve been very lucky that I’m able to discuss even mental health issues (ADHD) with mine and have them be willing to work with me, but I realize that’s very unusual.