Yesterday we briefly talked about Medicare Part A and Part B. Part A covers in-patient/overnight stays at the hospital while Part B covers most other services that involve interacting with other people. When Medicare started, prescription drugs weren’t a big cost driver. Basic drugs were available, they treated most common cases to some degree of effectiveness and unsusual cases were out of luck. And then drugs got expensive as they got more complex and the US patent regime encouraged non-market pricing of drugs. Additionally, the US Congress also discouraged non-market pricing of drugs as the federal Medicare program is not allowed to use the simple fact that it is the biggest buyer of medical supplies in the world to get a good price. Drug costs for old people became a massive political issue.
And thus an opportunity for Republicans in 2003 to do two things. The first was to offer a solution that emphasized “compassionate conservatism” for old people to help them get their drugs. Secondly, it was an opportunity to shovel a massive amount of money at drug companies without asking for a whole lot in terms of policy concessions. Thus Medicare Part D was born.
The initial design of Medicare Part D was a kludge of managed market competition. Private insurers offer plans that cover a variety of different drugs according to a basic benefit design. Companies could offer limited lists of covered drugs (formularies) or expansive (and expensive) lists of covered drugs. They could create two tiers (generic and brand) or seventee tiers of coverage with different co-pays and cost sharing. They could decide to require that all beneficiaries try Drug X before they would authorize Drug Y. The rules and plan requirements for Mayhew Insurance would be diametrically opposed to the rules for Big Blue Drug Value Super Duper Plus.
There are common benefit design elements for the individual beneficiary responsibility of costs. The individual would be responsible for a medium sized deductible of roughly $250. After that, the insurer would pay 75% of the contracted costs until the donut hole started at $2,250. From $2,250 to $3,600, the individual was responsible for all of the cost. After $3,600 in total drug costs, the insurer would pay roughly 97% of the remaining drug costs.
Compared to the previous Medicare drug benefit of almost nothing, Medicare Part D as originally designed was significantly better than nothing. It does provide some significant benefits to seniors while being confusing, complex and a massive give-away to drug makers as Medicare was expressly forbidden from getting good deals.
The Affordable Care Act made several signifcant technical changes to Medicare Part D. It still maintains the managed competition design but changes the payment structure. Over the long run, the goal is to get rid of the donut hole completely while in the short run, the goal is to minimize the out of pocket expenses for seniors who are still stuck in the donut hole.
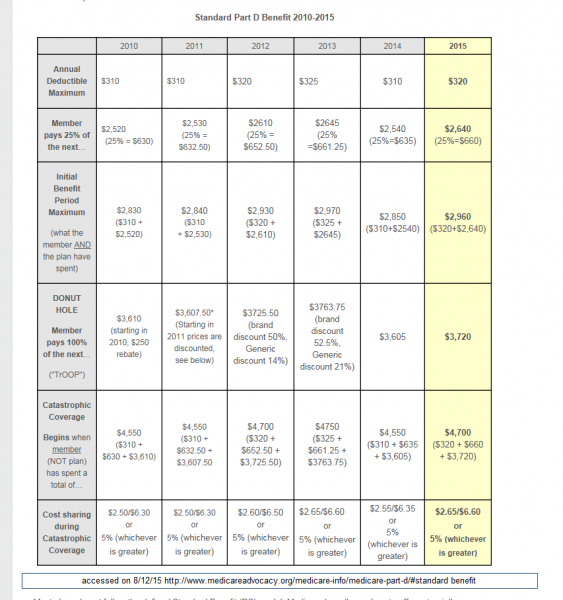
The Center for Medicare Advocacy has a good chart that describes how the benefit design is changing over the course of time.
For 2015, there is a $320 deductible. After that there is a 25% co-insurance until a total of $2,960 is spent (including deductible). The donut hole is for the next $3,720 in contracted rate spending. In reality, the ACA applies a roughly 50% discount to that $3720, so the individual will spend about $1,900 in the donut hole. After that catastrophic coverage kicks in and the insurer pays 95% of the costs.
There is no out of pocket limit. A retired hemophiliac with a million dollar a year drug claim will still be on the hook for $50,000 in drug costs under a Medicare Part D plan. That is an extreme outlier but it is a real case. A more realistic scenario would be someone on an anti-inflamatory drug plus an arthritis medication plus one of the new cholestral pills could easily see out of pocket costs of $4,000 to $6,000 per year even with their Medicare Part D policy.
Over the long run, the donut hole will disappear in 2020 due to PPACA, so out of pocket expenses for all seniors will stay the same or decrease but the drug coverage is not great for people who have very high cost prescriptions due to the lack of out of pocket maximums. A PPACA Exchange plan caps out of pocket expenses at a combined medical/pharmacy/surgery maximum of $6,500 per year. Medicare does not provide that type of protection.

Soprano2
Run those numbers for insulin injection pens with four or five other meds and I bet they’re higher. I was shocked to find out that there is no generic form of insulin available for my husband to purchase, because after finding out how much those pens cost once he’s in the donut hole (which happened in August this year) he asked the doctor. I think the pricing of insulin is a good example of how drug companies rape people who need what is literally a life-saving medication that has no substitute. I’m sure there are people who need insulin who don’t take it due to the expense. It’s shocking that a medicine that’s been around for 100 years still costs so much.
Richard Mayhew
@Soprano2: There was a great comment by one of our MD readers on insulin a couple of months ago:
Kylroy
@Richard Mayhew: So is the insulin my grandmother took in the 1990s markedly worse than what’s on the market now? Patents on medications last 10 years, right? Is the simple manufacture of insulin so expensive that producing 2005-vintage insulin would not result in significant cost savings?
pseudonymous in nc
@Soprano2:
To be fair, modern insulin largely better for diabetes management than the animal insulin that was used until the 1980s. It is also not cheap to produce, but cheaper now than when it was a choice between beef or pork insulin. (The pricing of test strips, on the other hand, is outrageous.)
Of course, in countries with actual healthcare systems, insulin (esp. for T1Ds) tends to be covered in full, because it’s considered better to pay for diabetics to manage their condition than for them to be priced into hospital.
Richard Mayhew
@Kylroy: That is outside my realm of knowledge — I don’t know anything relevant on the clinical side of medicine except incidental knowledge.
pseudonymous in nc
@Kylroy:
First of all, it’s not insulin, it’s insulins: some fast-acting, some long-acting. If you don’t respond well to one fast-acting insulin (say, Novolog) then you have Humalog or Apidra as other options. Options matter for diabetes management, which is an imprecise science at the best of times.
To some extent, it’s like asking why you can’t buy a new iPhone 3G for $10.
bvernia
Thanks for the explanation, Richard. Question, though: you say that in the catastrophic coverage zone, the insurer pays 95%. I thought that Medicare is the reinsurer for Part D plans, and so pays the majority of the costs in the catastrophic zone. The situation is further complicated in the case of low-income beneficiaries, for whom Medicare may pay significant costs, including in the donut hole.
japa21
One cost not factored in is the cost of the premiums for coverage. Plan D coverage is all over the place depending on plan. For my wife, it is $1,200 per year (approximately). Of course, when you get into Medicare Advantage plans, this is another thing that will be looked at as most of those include drug coverage.
One of the other issues with Plan D, and you alluded to it, is that the plan structures can vary widely. Some plans will work to avoid covering some people due to the tier structure they use for certain drugs.
japa21
@bvernia: Several states also have assistance plans for low-income seniors. Illinois provided assistance for my mother-in-law to the point where the most she ever paid for a prescription was $5.
Richard Mayhew
@bvernia: Yep, and you are bringing a lot of extra and needed complexity to the equation.
From the beneficiary side of the equation, they don’t really care if their insurer is the final payer or the feds are the final payer on the 95% of the catastrophic coverage.
And yes, on the premium side, there are several assistance programs (most notably, the Low Income Subsidy (LIS) program that helps reduce costs for people with low incomes). More on that probably next week (as well as the PACE program that I’ve been asked about several times)
skerry
Gentle reminder: Not all people using Medicare are seniors. Don’t forget those of us who are disabled and under age 65. There are some differences between the benefits this group is entitled to and those for people over 65 years old.
MazeDancer
Richard, what about the penalty for not buying a Part D?
People who take no prescription drugs still have to buy a Part D or they face a big, lifetime penalty if they wait. There are not that many good options for Part D. Either give your money to Wal-Mart for about 15 bucks a month. Or give $35 bucks a month to someone else.
It is, as you note, such a big giveaway to Pharma. Including how big the penalty is for not buying.
Interestingly, not much yelling happened by GOP about the “mandate” and “penalty” involved in Part D give-away when it was inacted.
But what do you advise people who take no drugs – or take drugs not covered by the formulary, Nature-Throid or some kind of not synthetic thyroid drug, for example – to do about Part D?
Richard Mayhew
@skerry: I really don’t have enough knowledge to comment too much on the benefit differences between Medicare for 65+ and Medicare for long term disability. Do you have good resources for me to look at?
skerry
@Richard Mayhew: Unfortunately, I don’t have a good resource. I have been educated only by walking through the minefield.
The most substantial difference I know of concerns Medigap policies. Federal law does not require insurance companies to offer Medigap to under 65ers. It is covered (or not) by state law. My state (Maryland) requires companies to offer only Medigap-A (the lowest level of supplemental coverage) if they offer coverage options to 65+.
Kylroy
@pseudonymous in nc: Okay, so it’s a range of options. My point stands: assuming 10 year long patents on drugs, why is generic production of 2005 insulins not happening? Is the simple fabrication of insulins so expensive that the cost savings from not paying licensing is negligible? Is it that nobody’s willing to buy a “second best” medication? Or just that nobody wants to produce one?
I’ll concede that the insulins are getting better, but it’s not like 2005’s options were leeches and bleeding.
Kylroy
@MazeDancer: As someone who administered Part D from 2006 to 2014, I’d advise you to buy the absolute cheapest plan you can find. That will provide you some coverage in case your medication costs spike mid-year, in which case you can then move to a more comprehensive plan come open enrollment.
The penalties, incidentally, amounted to about 30 cents additional monthly premium per month uncovered. The maximum penalty anyone was paying in 2014 was about $20 a month.
MazeDancer
@Kylroy:
Thanks for advice about “just go cheapest” on Part D.
Know many people who are trying to figure out what to do. Including computing out the penalty costs vs. not buying costs. And people who don’t live anywhere near a Walmart – yes, plenty of lovely villagey or rural areas with no Walmart – also have inconvenience factor of having to mail-order if they ever need to use.
Walmart-based policy is the cheapest. Difficult to send money to Walmart. But at least they came around on Marriage Equality.
elboku
As someone under 65 and disabled with MS, medicare prescript is useless for my newer drugs. The price is just way out there. And thanks to the feds, I cannot get help from the manufacturer. Due to my adult kids working and living with me, my household income is too high for other help. So, when I wind up in the hospital earlier, everyone will be paying thousands a day for my stay instead of paying for a drug to keep me OUT of the hospital.
Smart….
Mnemosyne (iPhone)
@Soprano2:
I have to say that, overall, our entire system penalizes people who were unlucky enough to be born with a chronic condition. Mine are fortunately fairly mild (asthma, ADHD, and rosacea) but it really sucks knowing that I have to pay for medication for the rest of my life and be subject to the whims of the pharma companies.
I haven’t used my preferred rosacea cream (Noritate) in over a year because the price for a small 25g tube has gone from $150 to $1,000. No, that’s not a typo. I don’t know what the hell they’re doing to make it so expensive, but I need to find something else (askew was telling me about Soolantra, so I’ll have to ask my doctor).
jl
@Richard Mayhew: that was my comment and I R economist FUD, not an MD. I am a doctor, but not a ‘real’ one. But if an MD who knows more about insulin story comes by, would like their input on the patent issue.
Edit: and thanks for an informative post. Except I think you meant to say that Congress encouraged non-market pricing, not discouraged, or maybe I misunderstood.
Edit2: not sure if in same comment, but simply adding clinically significant benefit is not a good economic rationale for granting a patent. If the incremental developments in insulin are fairly safe investments, that is, the probability of R&D investment success in making an incremental improvement is close to one, then funding those improvements through patent is not economically efficient. So, it is not clear that insulin pricing due to patent protection is efficient way to go. That is, patients may be paying too much for the improvements.
Salishness
OT but hopefully interesting development re coercive health screening for insurance. MrsNess recently moved jobs from a tech company to an established industrial conglomerate with a very old school paternalistic ethos. The insurance plan offered via Cigna is a high deductible HSA plan with all the attendant joys that implies.
But recently we received notice that all employees and insured spouses have to undergo biometric screening, presumably UAs, for undeclared smoking or face a $1500 annual insurance penalty. I’m wondering if this is common practice and whether the coercive aspect of this “request” is unique to this employer/insurer mix. I’d honestly be surprised if there were enough furtive smokers out there to make this policy worthwhile. Thoughts?
jl
This is a speculation on my part, I’d need to study the details of the benefit design more and think about it, but I wonder if part of the rationale for design of Part D was to allow consumers to reveal their demand through choice of part D plan, that is help the drug companies implement something closer to perfect price discrimination. Which would result in larger transfer of funds to big pharma, and suck more welfare benefit from consumers.
There might be some welfare improvement along one dimension, which is that consumers could choose benefit plan annually, so they would be less exposed to unexpected drug costs due to unexpected health events after the first year.
There was also another gimmick that seems very minor and tiny bore to me, but the price index used as a benchmark price favored large wholesalers, and there were claims it but serious squeeze on smaller firms. That would reduce prices, but seems to me it would be such a minor factor, price control could not have been the main rationale.
jl
@Richard Mayhew:
” And yes, on the premium side, there are several assistance programs (most notably, the Low Income Subsidy (LIS) program that helps reduce costs for people with low incomes). More on that probably next week (as well as the PACE program that I’ve been asked about several times) ”
I look forward to that post. My belief is that these programs aid implementation of something close to perfect price discrimination by pharma companies. They are advertised as gracious and compassionate concessions to people who cannot afford medication. But after a patent is granted, offering price concessions down to marginal cost of production for those who cannot pay higher prices is actually the profit maximizing strategy. I think I emailed RM an article on price discrimination by Louis Phlips that explains how it works. But the drug companies have to target these price concessions carefully to screen out people who could actually pay more, otherwise the price discrimination scheme breaks down.
Thoughtful Today
Fixed this for you:
“The initial design of Medicare Part D was a kludge”The entire corporate insurance scheme is a kludge.
In hacker terms the corporate insurers are a “man in the middle” attack (MiTM). Insurers do NOT provide health care, they just leach out profit.
Please consider supporting Single Payer / “Medicare Part E (For Everyone)”. Bernie does ;)
Thoughtful Today
Fixed this for you:
“The initial design of Medicare Part D was a kludge”The entire corporate insurance scheme is a kludge.
In hacker terms the corporate insurers are a “man in the middle” attack (MiTM). Insurers do NOT provide health care, they just leach out profit.
Please consider supporting Single Payer / “Medicare Part E (For Everyone)”. Bernie does ;)
Richard Mayhew
@Thoughtful Today: Please go fuck yourself as you tear down the world without being able to answer some simple design quetsions about how to actually implement Medicare-E. My moral universe is to take a decent improvement that is a kludge instead of nothing that could be delivered by flying unicorns shitting rainbows out of their ass.
Please explain to me why, if Medicare-E is such a superior system that has no drawbacks, no trade-offs, no problems besides defunding corporate power why Vermont elected to pull its single payer waiver application.
Real policy is complicated, slogans are easy.
Marina
I hit the donut hole after my supplemental insurer spent $2,960 on my medication. I have to spend $4,700 out of pocket before I’m out of the donut hole. Gee, thanks George W.!
Drug costs have gone up so much so fast that people on Medicare, who used to hit the donut hole in the fall, are now routinely hitting it in early spring.
Reps from both my Part D insurer and my local pharmacy are telling me that sick people on Medicare start crying when they find this out. My insurance rep said she can barely stand her job anymore, because of all the crying customers. People are taking their meds every other day, or not taking them at all.
Phasing out the donut hole entirely won’t happen for at least five years (assuming a Dem becomes president). Jeb! has said on record that as president he would phase out Medicare. Why isn’t this news?
It’s more cost-effective for me to buy my meds from canadadrugs.com, which carries a generic version that’s unavailable in the U.S.
bvernia
At the risk of drawing the ire of @Thoughtful Today, Richard, I would be interested in your take (maybe in a separate post) on mergers and consolidation in health insurance companies, particularly those dealing with Medicare (Parts C and D and the ACA). I work on fraud cases (whistleblower and defense), including some in both Medicare Parts C and D, and it appears that CMS, which administers Medicare, seems to be following the lead of the Pentagon in the 1990s, and tolerating – if not outright encouraging – mergers in the interest of reducing the number of contractors with whom it has to deal. This would seem to undercut the supposedly beneficial competition on which these programs were sold. (Apologies if you’ve already written about this in another post.)
Richard mayhew
@bvernia: I am trying to put my thoughts together on health insurance company mergers. First, I’ll formed thoughts are in most markets not a bad thing for 2nd best economist/wonk pov as consolidated layers can get better rates from consolidated providers. See my posts GIni in a bottle for my mental model. PPACA lowered cost of entry for insurers and fragmented market power on payer side while providers are still consolidating.
Some markets where merged entity is too much of a market could be issue resolved by spinning segments off…. Not an antitrust lawyer, not a m&a finance geek either
Dennis Byron
This is a nonsense description of Part D of Medicare, both of its history and of its current structure.
Medicare Part D was signed in 2003 but it was not in any way, shape or form the first time the Federal government or Medicare itself paid for drugs. Part D is only involved in one type of drug: self administered. Part B of Medicare always did and still does handle the other type, the most expensive type of drugs, which are administered in a clinic or doctor’s office. All Part D did primarily was change a previous program through which self-administered drugs were paid for through Medicaid for the poor and through state programs, private gap or private retiree supplemental insurance for the middle class. Now instead – via a voluntary program – some of the middle class people can choose a Part of Medicare to get their drug coverage rather than depend on private insurance. They still pay a premium as they always did. Many of the state programs still exist. As for the poor, there is effectively no difference; instead of getting their self administered drugs free or nominally free through a joint state/Federal welfare program, Medicaid, they get their self administered drugs free or nominally free through a 100% Federal welfare program. But this is basically transparent to them
As for how Part D works today, there is constant negotiation involving the Federal government. But the negotiation also involves insurance companies and drug distribution channels as well as manufacturers. This approach has lowered overall government spending and the cost to beneficiaries (other than to the poor who never had to pay anything and still do not have to pay anything). Almost no popular Part D plan follows the so-called “basic benefit design” described here. Everything else described here accurately describes how Part D works. But it is also the way all drug plans work (for example, the drug plan people get from employees). There is nothing special about the way Medicare Part D works.
It is incorrect to say that current law eliminates the “donut hole;” all that happens is that the co-pay in the donut hole under the so-called “basic benefit design” (which is typically not used in popular plans) will in the future be the same as in the initial spend phase, 25%. Most analysis suggests that this will increase, not decrease the out of pocket expense – including premiums – for most people on Part D. However for the about 5% of people on Medicare who previously were affected by the donut hole (none of whom were poor because as noted above, under Part D, drugs are free or nominally free for the poor), their out of pocket expense will be lower (assuming the unlikely case that drug prices do not increase).
Chris T.
Minor note: it’s spelled “cholesterol”, with the “-ol” ending common to all alcohols. (Cholesterol is technically an alcohol.)
Soprano2
@Marina:
Another thing most people don’t understand is that the money you pay out-of-pocket counts toward the total amount that gets you to the donut hole.
Thanks for posting that explanation about the continuing development of insulin. I wish I understood why some drug manufacturer didn’t take advantage of the expiration of patent on not-that-old insulin to manufacture a generic version. There are enough people out there who can’t afford to buy insulin now whose lives would be improved by being able to afford insulin. For some the alternative is to not take the meds at all, and surely that’s not a good alternative for our health care system. Either we can pay now, with meds, or later with hospital stays and operations. We’re lucky that we can afford the meds, but lots of people wouldn’t be able to pay hundreds of dollars a month for insulin.