When should people get treatment? Should people get treated for something as early as possible? Or should they wait until later when discrete milestones are passed? What does the decision tree look like?
The Incidental Economist passes along the latest research on the prostate cancer treatment debate. The United States has a culture of treatment as soon as prostate cancer is bio-chemically detectable. Most of Europe has a culture of treatment at a milestone.
NEJM, Anna Bill-Axelson and colleagues published the latest findings from the Scandinavian Prostate Cancer Group Study Number 4 (SPCG-4).
RESULTS: During 23.2 years of follow-up, 200 of 347 men in the surgery group and 247 of the 348 men in the watchful-waiting group died. Of the deaths, 63 in the surgery group and 99 in the watchful-waiting group were due to prostate cancer; the relative risk was 0.56 (95% confidence interval [CI], 0.41 to 0.77; P=0.001), and the absolute difference was 11.0 percentage points (95% CI, 4.5 to 17.5)….
Aggressive treatment works in this care. However IE also passes along a critique of translating this research into the United States.
Second, the results of this study aren’t necessarily generalizable to a US population, as Richard Hoffman explained.
PSA screening became widespread in the US in the early 1990s—a decade before the first SPCG-4 publication. Perversely, the American way was to expend considerable resources to promote screening efforts to find cancers…before knowing whether these cancers could be successfully treated. [So,] the SPCG-4 results are not readily translatable to US practice. Only 5% of the study cohort had cancers detected by screening PSA—the rest either had symptoms and/or a palpable tumor. In the US, a substantial proportion of men with PSA-detected cancers have microscopic disease—which may never cause problems during a man’s lifetime. The US Prostate Cancer Versus Observation Trial (PIVOT) also evaluated surgery vs. watchful waiting. However, PIVOT, which mostly enrolled men with PSA-detected cancers, found no benefit for surgery. Post-hoc analyses suggested that only the small proportion of men with higher-risk cancers (based on PSA and the microscopic appearance of the cancer) seemed to have a survival benefit.
The US research has found that aggressive treatment of bio-chemically detected prostate cancer does not do much to improve outcomes for the general population of biochemically detected prostate cancer patients. Aggressive treatment tends to have significant side-effects as well.
What could a potential decision tree look like that minimizes overtreatment while also minimizing undertreatment?
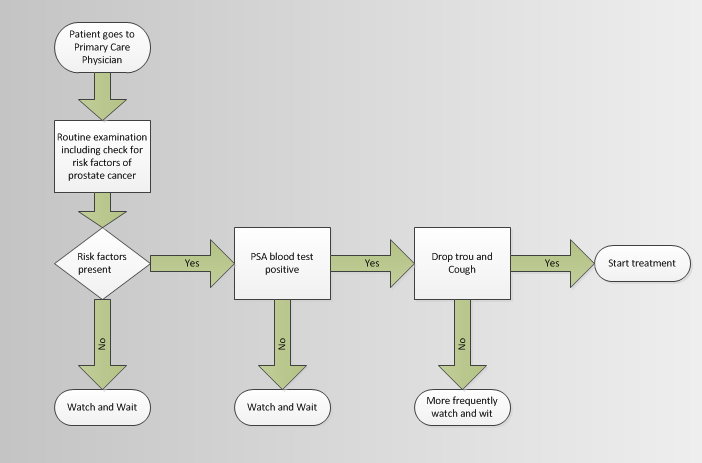
The goal is to treat only the cases of cancer that could actually kill someone. Treating a cancer that is localized and miniscule and only bio-chemically detectable exposes individuals to significant side-effects that will decrease the quality of their life without improving their long term survival probabilities. A 107 year old man would be a poor candidate for aggressive treatment of a biochemically detectable but not physically detectable cancer as something else is far more likely to kill him first. A 43 year old man who has a biochemically detectable cancer would benefit from aggressive watching and waiting as he avoids side effects for a while, but aggressive intervention can be performed if the cancer becomes more significant as that larger/more aggressive cancer would have a decent chance of actually killing him if left unchecked.
Moving back to the insurance company beat; insurance companies can use their purchasing power and benefit designs to enforce national best standards of care on their members. If the best standard of care is that aggressive prostate cancer treatment only is useful for physically detectable prostate cancers, the insurance company could choose to either not pay for or pay at a lower rate aggressive interventions of bio-chemically detected only cancers while paying full freight for physically detected cancers.
The big problem with the previous paragraph is that type of policy is guaranteed to produce amazingly sympathetic sob stories on the local news. Insurance companies like to avoid being the easy and accurate villian that is saying no to the cancer treatment of a well spoken, well connected middle age male. We’ll lose that PR battle every time, and if a single company in a market engages in best practices only payment models that involves saying no, they’ll quickly lose market share.

jayackroyd
I’m confused. Why would an examination for an enlarged prostate (that’s how I read “drop trow and cough”) come late in the game? Isn’t that part of a normal physical? Isn’t that less expensive (and apparently more effective by this decision tree) than the PSA test?
jayackroyd
Also, I think you might be misconstruing the battle–at least if the advertising on my local sports talk radio station is any indication. Seems to me this is another provider vs insurer battle, with the PPACA forces on the side of the insurer’s profits rather then the provider’s revenue.
Richard Mayhew
@jayackroyd:
Right now a physical check for an enlarged prostate is not an every well-visit function. It is cheap, it is fast, and it is reliable to say something is going on. And if it and the PSA are showing something, most likely there is something to do.
Richard Mayhew
@jayackroyd: Were insurance companies forcing best practices on providers pre-PPACA? No — a big part of that was a fear of being the villian of the sob story on the local news at 6, 10 and 11 tomorrow night.
Richard Mayhew
Here are the current guidelines for screening:
Richard Mayhew
@jayackroyd: And yes, I completely agree, the underlying argument is payer control versus provider/payee control. The inability to say NO means more money for providers.
Tommy
This conversation at many levels is above my pay grade. At one level I get aggressive treatment for a person 107 doesn’t make sense. I totally get we need to get our “arms around” what we pay for health care. That such large percentages of what we pay are for a small percent or two of folks at the very end of their life is troubling.
But IMHO this gets into the parking lot (not ballpark) of the “death panel” thing (and clearly I know these are a right wing fabrication).
I say this, cause well I always thought that you want to catch something like cancer as soon as possible. Treat as soon as possible, cause treatment sooner rather then later is “easier” as cancer treatment goes (and costs less).
Again maybe everything I know is wrong, but something about this just doesn’t compute for me.
jayackroyd
@Tommy: Sorry Tommy. It’s probably there if you click through, but the thing about prostate cancer is it is often very slow developing, and often not fatal. So the PSA test is, in a sense, too sensitive. Most men with positive PSAs will die of something else, so treating everybody for prostate cancer–with a treatment that has serious quality of life implications–is probably a bad idea. Aggressive treatment outcomes in the US are no better than wait and watch outcomes in the UK.
And wait and watch has no side effects and is way cheaper.
As Richard says, our news coverage doesn’t help us here–a dramatic outlier can become a news story. Or, as your comment demonstrates, the early detection story informs the understanding of “cancer” in a way that is not helpful here.
dnfree
“Watchful waiting” after an elevated PSA doesn’t consist of checking for an enlarged prostate. An enlarged prostate can be a different problem entirely. “Watchful waiting” means having a somewhat painful biopsy done through the rectum into the prostate. Doing that repeatedly causes its own set of complications. What they are looking for there is how much cancer and at what level. But of course the biopsy could miss your cancer entirely. It’s a difficult decision.
You get a T score, a Gleason score, and other scores and then try to make a decision based on those.
http://www.cancer.org/cancer/prostatecancer/detailedguide/prostate-cancer-staging
jayackroyd
@Richard Mayhew:
Right. I almost wrote that in my comment–the PPACA is supposed to help reduce overutilization costs by outcomes research and (effectively) changes to reimbursement practices.
jayackroyd
@dnfree: Thank you!
raven
@jayackroyd: My fitness oriented friends and I have been told that probably IS what we will die of since we’re taking care of other functions through diet and exercise. At 64 it will be a while but, still.
Tommy
@jayackroyd: I am blessed that literally no family members of mine have had cancer in my lifetime. So my knowledge here is limited. I guess I need to do some research on prostate cancer, cause I am getting to the age, and now I have a plan through the ACA where as I understand it an exam would be free, it couldn’t hurt to get one.
Clearly not something I am looking forward to :). But as I mentioned and think, prevention and early detection of a problem is a good idea.
Finally I am kind of behind the thesis in what Richard wrote. I get stats. And I think the quality of life is important when thinking of treatment. I realize a TV show isn’t reality, but Showtime had a show on called the Big C that dealt directly with “quality of life” in a manner I felt very compelling.
Gin & Tonic
@Tommy: Clearly not something I am looking forward to :)
Jeezus, don’t be a wuss. A digital rectal exam takes 10 seconds. I’m sure you other more uncomfortable things every day of the week.
jayackroyd
@Tommy: I guess I was talking about the idea of “the big C.” Cancer isn’t one disease that happens to break out in different places. It’s a host of different diseases that manifest themselves by inappropriate reproduction of cells. The great success we’ve had with early detection of some cancers doesn’t mean that early detection is a panacea–especially as tests get more sensitive.
The positive public health benefit of early detection campaigns isn’t helping public awareness of prostate cancer treatment. Providers’ pushing treatments through advertising don’t help.
dnfree
@raven: Sadly, we know more than one really fit person who eats well and has developed prostate cancer in their 50’s or even 40’s, and those do tend to be the aggressive cases.
aimai
@Tommy: Yup, everything you know is wrong. Not a death panel issue.
raven
@dnfree: Well maybe that’s what the doc meant since we are mid-60’s.
Gin & Tonic
@Tommy: People are beating around the bush with this “quality of life” phrase. After most aggressive prostate cancer treatment most men can’t get it up any more. Is that something you want to give up, if you weren’t going to die soon anyway? Sure, pancreatic cancer kills you quickly and certainly; prostate doesn’t.
Tommy
@Gin & Tonic: Oh it is more of just a running joke I see in like every sitcom on TV. I am sure I can make it through it.
rikyrah
Look men…get that PSA test. Period.
Tommy
@Gin & Tonic: I admit often there is a lot I don’t know. My family has NO history of cancer. Two friends parents had pancreatic cancer, so I guess the speed with they passed away taints my views of all cancer, when reality might be something different (and yes I know that is a terrible, terrible kind).
raven
@rikyrah: And a goddamn colonoscopy. I delayed my last one because I had a thrombosis hemorrhoid that came along with a nasty case of diarrhea. I kept saying ” I don’t want to do something that induces THAT so I waited a year. When I did it 2 months ago I prepared with ah low fiber diet for 4 days and it was a breeze.
JCJ
@Richard Mayhew:
Good morning Richard. I think a very important distinction to make is what is involved in “watchful waiting.” I have not yet read the NEJM article, but I recall a study that was essentially surgery vs observation for prostate cancer. This is not the same as watchful waiting in the form of “active surveillance.” Here is a PubMed link
http://www.ncbi.nlm.nih.gov/pubmed/22453335
Curr Opin Urol. 2012 May;22(3):222-30. doi: 10.1097/MOU.0b013e328352598c.
Active surveillance: the Canadian experience.
Klotz L.
Author information
Abstract
PURPOSE OF REVIEW:
Active surveillance has evolved to become a standard of care for favorable-risk prostate cancer. This article is a summary of the rationale, method, and results of active surveillance beginning in 1995 with the first prospective trial of this approach.
RECENT FINDINGS:
This was a prospective, single arm cohort study. Patients were managed with an initial expectant approach. Definitive intervention was offered to those patients with a prostate specific antigen (PSA) doubling time of less than 3 years, Gleason score progression (to 4 + 3 or greater), or unequivocal clinical progression. Since November 1995, 450 patients have been managed with active surveillance. Median follow-up is 6.8 years (range 1-16 years). Overall survival is 78.6%. Ten-year prostate cancer actuarial survival is 97.2%. Five of 450 patients (1.1%) have died of prostate cancer. Thirty percent of patients have been reclassified as higher risk and offered definitive therapy. The commonest indication for treatment was a PSA doubling time less than 3 years (48%) or Gleason upgrading (26%). Of 117 patients treated radically, the PSA failure rate was 50%. This represents 13% of the total cohort. Most PSA failures occurred early; at 2 years, 44% of the treated patients had PSA failure. The hazard ratio for nonprostate cancer to prostate cancer mortality was 18.6 at 10 years.
SUMMARY:
We observed a very low rate of prostate cancer mortality in an intermediate time frame. Among the one-third of patients who were reclassified as higher risk and retreated, PSA failure was relatively common. However, other cause mortality accounted for almost all of the deaths. Further studies are warranted to improve the identification of patients who harbor more aggressive disease in spite of favorable clinical parameters at diagnosis.
PMID: 22453335 [PubMed – indexed for MEDLINE]
Fair Economist
I’m very aware that the US probably overtreats prostate cancer – but – in that Scandanavian study 2/3rd of the people who would have died of prostate cancer did anyway even with treatment. That means either treatment is happening too late or they’re doing inadequate treatment (e.g. radiation rather than excision).
a hip hop artist from Idaho (fka Bella Q)
@jayackroyd: I’ll even risk offering this: even in breast cancer, there are a variety of different kinds. Some are slow growing, some are aggressive and dangerous. The public awareness campaigns around the pink ribbons may well have created a culture of fear about breast cancer(s) that means overtreatment of cancers that are not aggressive.
It’s not a popular position to state, as there is a lot of emotion around it. But, that doesn’t make it inaccurate.
Ruckus
Using the example of prostate cancer screening I have a little experience.
At about 45 yrs old, during my standard annual physical my PSA was wildly elevated. I had to undergo an ultrasound(an insertion inspection) which in of itself is no big deal. But it took 4 months and 2 different drugs and that to find out that it was an infection, not cancer. That was the scariest 4 months of my life. Talk about a mid life crisis. Could it have been avoided? Should it have been avoided? Would I have been better off? Will never know, that’s not how it worked out. Is there a better way? Sure sounds like where we have gotten to today is better.
Cancer may be insidious but it isn’t smart, we can be.
JCJ
@Fair Economist:
Excellent point. Hormonal ablation plus radiation is much more appropriate treatment either alone or following surgery than just surgery alone for locally advanced disease.
mellowjohn
my father had prostate cancer at the age of 68, so my primary care doc started checking me almost immedately. never had an elevated PSA, but about 5 years ago during my annual Px, he found a lump and sent me upstairs to a urologist. he did a biopsy that proved negative, but started checking me every 6 months. two years ago last december – just after i’d turned 65 – he found another lump. i still had a very low PSA and a very small prostate, but a biopsy came back positive with a Gleason score of 7. did 45 sessions of proton radiation, April thru June 2012.
saw the urologist yesterday and my PSA is “undetectable” and my prostate is so small he said he had trouble finding it.
YMMV, but i feel great, everything still works fine (thank you very much!) and i’m all for early treatment.
p.s. when i was still in the “what-the-fuck-am-i-gonna-do” stage i read a NYTimes op-ed by zeke emanuel (brother of my hated mayor) arguing against proton radiation therapy, saying it hadn’t proved more effective than other kinds of treatment for prostate cancer. i told my wife at the time that i was looking forward to the op-ed he’d write after he’d been diagnosed with it.
scav
@a hip hop artist from Idaho (fka Bella Q): If I understood some earlier reserearch about breast cancer correctly, out ability to “detect” it has so outpaced our understanding of how it actually progresses (or even if it progresses and what that seems to influence all the alternative outcomes, there’s a lot of idiosyncratic in medicine that hasn’t been broached) it may be totally messing with survival statistics. Some cancerous whatevers do seem to just mistappear or never go anywhere or do much. But, by agressively going after all the earliest signs, we’re lumping in all the ‘naturally’ occuring non-progrssions with the ‘cures’ and so the survivial rate as measured hasn’t budged as much as we would expect. And’ it’s messing with our understanding of what actually helps and is going on.
Joel
Just a nit, but biochemical is one word.
Wow, you fixed that fast.
Bobby Thomson
@Gin & Tonic: Isn’t John Kerry a prostate cancer survivor?
CONGRATULATIONS!
The chemo for prostate cancer treatment, combined with an inept nurse who put the wrong kind of dressing on his hand, is what killed my grandfather.
He bled to death. Blood couldn’t clot, skin couldn’t heal over the hand wound because of the chemo. Took about two months.
Gotta be a better way. Fucked if I know what it is.
jayackroyd
@rikyrah: My doctor and I talked it over, and I declined.
jayackroyd
@a hip hop artist from Idaho (fka Bella Q):
Yes. I almost included a sentence or two about preventative mastectomy, where a genetic marker is the very sensitive test for one kind of very aggressive, early developing breast cancer.
So it’s not even right to talk about “breast cancer” as a single disease. This is not to say that the early detection public health efforts have not been really valuable and successful, but that one result of research and treatment experience is that it is not sufficient.
jayackroyd
@a hip hop artist from Idaho (fka Bella Q): I was talking about some of these issues with the doctor who was treating my broken wrist. (Yes when I visit doctors i talk about health care policy.) He remarked that people don’t really understand that medicine isn’t really science–it’s accumulated folk wisdom. Actual advances come from trying stuff to see if it works on a patient who won’t be made worse off if it doesn’t. This in the context of advances in hand transplant techniques. One only does a hand transplant on someone missing both hands, for instance.
So aggressive treatment for all cancers was the default until outcomes made it clear that this wasn’t really the best idea. Radical mastectomies got replaced by lumpectomies and then by radiation only. But public awareness lags….
Mandalay
I have had two prostate biopsies following very high PSA counts. The results were negative (i.e. good). Then I read the small print which nobody had told me: ejaculation within 24 hours prior to taking the blood test will increase the PSA count.
Since then I make sure to behave myself for a day or two before the blood test, and all has been well with my PSA count. It’s crazy that I wasn’t cautioned about this by anyone involved. Assume that doctors are busy and forgetful, and won’t necessarily tell you everything you should know. Research, and challenge what they tell you if appropriate. And thank heavens for the intertubes which let us easily check up on stuff ourselves.
p.s. And while the prostate biopsy is certainly undignified, it is also a complete nothingburger. Zero pain during or after, and I was driving home 15 minutes after the test. Men really need to get over worrying about people messing with their ass when cancer is a possibility.
Mnemosyne
@dnfree:
This does seem to be a variable that was left out — as with many cancers, the younger you are, the more aggressive it tends to be. So prostate cancer in a 45-year-old will probably need to be treated sooner than prostate cancer in a 75-year-old.
I had to get my baseline mammogram around age 35 because my mother died of breast cancer before she was 40 (though I now suspect that it was due to x-ray exposure as a dental hygienist — they weren’t nearly as careful about radiation exposure in the early 1960s as they are now).
Wag
@rikyrah:
Or, better still, not.
The United States Preventive Services Task Force is a governmental agency charged with analyzing ALL the available data about preventive medical procedures, and then coming to a scientific consensus about whether treatment following a positive screen saves lives, and whether the benefits of a treatment outweigh the risks of complications following a treatment.
Screening procedures are graded A through D.
Grade A recommendations are screening procedures where early detection saves lives, improves outcomes, and saves money. For a 55 year old, these tests include Colon cancer screening, Pap smears for cervical cancer screening, blood pressure screening, cholesterol screening, and HIV screening.
Grade B recommendations are procedures where, on the balance, we save lives, but at a risk of higher false positive tests, so the benefits aren’t quite as strong as Grade A recommendations. Grad B tests are clearly worthwhile. For a 55 year old, these tests include screening for depression (if the clinic has a structured follow-up plan) and for alcohol abuse, mammography, diabetes screening, and screening for sexually transmitted disease in at risk populations. Lung cancer screening in patients with a 20 year smoking history is a new recommendation in this Grade.
Grade C recommendations are procedures where there may be benefit for a small segment of the population, but on balance, these services should not be recommended. For a 55 year old, these services include depression screening in the absence of a structured depression follow-up plan.
Grade D recommendations are procedures where harms from treatment outweigh the benefits of screening for and treating the condition. screening procedures that fall under this grade include PROSTATE cancer screening, ovarian cancer screening, pancreatic cancer screening, and screening for carotid artery disease.
From the USPSTF website with regards to prostate cancer screening
The medical societies that urge all men to get screed for prostate cancer (American Cancer, American Urology, etc.) all have a vested financial interest in the treatment of pros tae cancer, and are part of the prostate cancer industrial complex. Be wary of their recommendations and their cherry picked data
Mandalay
@Wag:
I think you are confusing the PSA test with the prostate biopsy.
The PSA test is simply an analysis of your blood used to assess the relative probability that you may have prostate cancer. The test is in no way definitive.
The prostate biopsy is the procedure that involves putting equipment up your ass to extract tiny pieces of your prostate for analysis to determine whether you may have prostate cancer. That examination is frequently performed based on the results of your PSA test.
You may or may not have a point about the “prostate cancer industrial complex”, but urging people not to even get a blood test is very bad advice.
CONGRATULATIONS!
@Wag: Both my “insurance doctor” and the old family friend doctor – the guy who I see when something has gone really wrong – do not believe that the PSA test is in any way, shape or form useful.
Both docs happen to have a pretty elderly clientele, I’m one of the youngest patients. They have pretty extensive experience with prostate cancer. I trust their diagnostic abilities more than a single test result. Which is how it is supposed to work!
Wag
@Mandalay:
Did you even read the bulk of my comment, or click through on the link that I provided?
I’m a physician who knows full well that PSA is a blood test, not a biopsy. PSA testing is an inaccurate and insensitive test that leads to unnecessary biopsies which finds slow growing tumors that will never hurt my patients, leading to unnecessary surgeries and/or radiation therapy, and unnecessary complications related to the unneeded treatment.
Aggressive prostate cancers tend to be metastatic at presentation, and screening doesn’t do any long term good for them, either
The USPSTF fully backs me up on this. Please see my link above.
Mnemosyne
@Wag:
My husband’s father was diagnosed with an aggressive form of prostate cancer at age 64. So your recommendation is that my husband ignore the “cherry-picked data” and refuse to get a PSA test because it’s totally useless for everyone?
Wag
@Mnemosyne:
In families with a strong family history of prostate cancer, the curves are completely different. My brother in law’s father and 2 brothers have all died of prostate cancer. For him, screening makes total sense. For the average risk patient, not at all. For your husband, probably somewhere in between. Your husband should have an informed discussion with his physician about the risks and benefits of screening.
a hip hop artist from Idaho (fka Bella Q)
@Wag: I’m hoping that you can at least understand my decision to forego that feminine rite of passage commonly known as the baseline mammogram, even if it would not be your recommendation. There is absolutely zero history of breast cancer in my maternal line (or paternal, for that matter). I believed 20 years ago that mammograms caused more agony than they prevented. And that’s before you get to tx of a malignancy, or whether DCIS should be be treated or watched first.
I’ve seen women stress for weeks over a shadow that on biopsy turned out to be not cancer. My ob-gyn still gives me a script for a mammogram and says “I know you won’t get one, but I need to chart this.” Last year he just handed it to me and said “I’m more comfortable with your adamant position now than I was 20 years ago, but I still have to recommend…”
Mandalay
@Wag:
Yes, and I am already well aware of the debate.
Yet your comment explicitly advised against getting the blood test, which would precede any biopsy.
It necessarily leads to some unnecessary biopsies, but it will also lead to some biopsies that are worthwhile. I have been down this path myself, and have twice elected to take multiple PSA tests (three tests on one occasion, two on another) in case the results of one PSA test were inaccurate, yet they all came back with very similar results. The process of counting from a sample is of course inherently inaccurate, but that does not make it highly inaccurate, or inherently worthless.
I see no good reason to generally advise people against getting a PSA test, which is what you did. The debate should be on how to proceed once the PSA test results are known, and this will vary based on all kinds of factors, including the patient’s age and medical history. I share your skepticism about the readiness (eagerness?) of doctors to perform biopsies, but that is an issue distinct from the PSA test.
Wag
@a hip hop artist from Idaho (fka Bella Q):
I recommend mammograms, but completely understand your viewpoint, and tell my patients who are like you exactly what your doctor tells you. You have made an informed decision,
In addition, the evidence pretty clearly shows that every other year mammograms are as effective as annual.
And for my male patients who still want PSA testing, i do offer the test after they make an informed decision about eh risks and benefits. It is only a minority of men who opt for testing, but I still do it.
Wag
@Mandalay:
Please click on this link and read the recommendations from the USPSTF. Perhaps then you’ll understand my reluctance to recommend testing. In particular, read the evidence report, which you can access near the lower right part of the page
http://www.uspreventiveservicestaskforce.org/prostatecancerscreening.htm
Kylroy
@Wag: This whole issue absolutely reminded me of Medicare’s switch to only providing biannual mammograms. It’s precisely the kind of wise, largely money- and pain-saving high level policy decision that is also *guaranteed* to get an insurance company in deep trouble. Because the thousands of people who saved themselves money and pain by halving their mammogram visits are not going to be on the nightly news or the front page, but the one person whose doctor says her cancer would have been treatable if detected a year earlier absolutely will be.
WereBear
@a hip hop artist from Idaho (fka Bella Q): You are utterly correct. In fact, a big study came out last fall (and was mostly ignored by the MSM) about the over-treatment of breast and prostate cancers.
This isn’t just wasted dollars, it’s eroded quality of life.
And since treatment itself is carcinogenic in many cases, it’s also dangerous.
WereBear
@a hip hop artist from Idaho (fka Bella Q): Me too!
I finally broke down and got one. It turned out to be totally useless. I have a structure that doesn’t work well. I just refuse now; no point in irradiating an area for nothing.
CONGRATULATIONS!
@WereBear: Preach it. I don’t buy the “fifty percent of all cancer deaths is from chemo” thing I’ve been hearing – but chemo killed both people who I have personally known with cancer.
Wag
@WereBear:
This.
Mandalay
@Wag: Yes, I have seen that before, and I still do not understand the opposition to the PSA test for older men. Pulling a sample of blood from my arm will not harm me, and for all its limitations I do not view the PSA count value as worthless or meaningless. I am glad that my doctor has a history of my PSA count (which has significantly decreased).
As I said before, it’s what we do with the information that the PSA test provides that should be contentious. I am much more concerned about the possible harmful effects of repeated prostate biopsies, and any insights you have on that would be welcome.
Wag
@Mandalay:
With each prostate biopsy there a small but real chance of infection and bleeding. Also, keep in mind the prevalence of clinically meaningless cancer. By age fifty, 50% of men will have a small focus of clinically meaningless prostrate cancer. At age sixty, 60% will have cancer. Each biopsy increases the risk of finding one of those clinically meaningless cancers and prompting clinically harmful and unnecessary treatment.
a hip hop artist from Idaho (fka Bella Q)
@CONGRATULATIONS!: Even when not deadly, chemo makes life suck for the time people are getting it. It’s a quality of life thing – to think that people are getting surgery and chemo for a condition that might never get worse is horrific.
I recognize that it’s not exactly easy to tell which specific growths will grow and/ or spread, but I think people have been conditioned to expect really aggressive treatment, period the end. And the omnipresent pink “get your mammos and get them often” campaigns can have some real downsides given that.
Mandalay
@Wag: OK, thank you.
azlib
I am a prostate cancer survivor. I had robotic surgery a little over a year ago after having a rising PSA level which finally went over the screening limit. A biopsy revealed the cancer. I did my due diligence and was aware of the screening controversy. I elected surgery because I am 63 and in very good health and have a potential life expectancy of 25 to 30 years.
Yes, there are side effects (impotence and incontinence), but my good health and an excellent surgeon mitigated those risks and the symptoms are mostly gone after a year. If I had been 10 years older or in poorer health, I would have likely chosen watchful waiting. So the decision tree is also based on age and health.
Another factor to keep in mind is you typically do not die of in situ prostate cancer. You die of bone cancer, since metastatic prostate cancer has a bone affinity. Bone cancer is very painful and not a pleasant way to go.
FInally, there is a problem knowing which form of prostate cancer you may have . Most forms are very slow growing and will cause no problems in a person’s expected lifetime. Others are very aggressive. Unfortunately, the current tests cannot tell which is which.
It is likely I had a slow growing form of cancer. Statistically, I had a very good chance of dying of something else. But when push came to shove did I want to take that chance.
TriassicSands
@jayackroyd:
I’m not sure that is true; and stating it that way is probably misleadingly simplistic. Further, it is difficult to compare the statistics in the UK and US, at least in part because of the widespread use of PSA testing in the US and the earlier diagnosis in this country.
Watchful waiting is an older term, and “active surveillance” is a better and more accurate description of the general alternative to aggressive treatment.
As a radiation oncologist once told me, “We (the US) are almost certainly overtreating prostate cancer. The difficulty is in knowing which cancers will cause a premature death and which will be present for years in patients who die of other causes.”
Unfortunately, our ability to differentiate is not very good, because of the uncertainty of the variables involved.
A couple of years ago there was an OP-ED in the NY Times by the doctor who had developed the PSA test. He wrote that, in his opinion, it was being overused and leading to unnecessary treatment. However, if one waded through the first three quarters or so of the essay, one arrived at some crucial information — those who have family members who have died of aggressive prostate cancers should ignore all the previous caveats and have regular PSA tests.
Prostate cancer is a tricky disease. Death from prostate cancer can be very ugly. It commonly metastasizes to the bones and that is extremely painful Nearly 30,000 American men die each year from prostate cancer, which is now almost 10,000 fewer than the number of deaths from breast cancer. If I’m not mistaken, the two statistics used to me much closer.
The percentage of men who survive 5 years after diagnosis is 99.2%. That sounds great. But my father was diagnosed with metastatic prostate cancer in 1984 and he made the five year survival milestone.. However, he died a very painful and miserable death in 1990, a few months short of six years after diagnosis. Once the cancer escapes the prostate gland, you get treated, not cured. Depending on your age and other health considerations, you are likely to die of prostate cancer.
However, his was a relatively aggressive cancer. I don’t know what his Gleason score was, but for patients with a Gleason score of 6 (3 + 3) or below, active surveillance may well be an option. For those with scores of 8 and above, the likelihood is the disease has spread beyond the prostate gland and all that can be done is managing the disease, as in the case of my father (hormone therapy). The real problem Gleason score is 7. There are two forms of Gleason 7, and I’ve read conflicting reports about their relative importance. The first number represents the degree to which the most common cancers cells in the gland are different from normal cells. The second number is the degree to which the second most common cancer cells in the gland are different from normal cells. Initially, I read that a Gleason 3 + 4 has a statistically significant better outlook than does 4 + 3. However, more recently, I read something that cast doubt on that.
Like so much about this (and other) cancer(s), there is much we still don’t know.
Yes, the after effects of prostate cancer treatment can be unpleasant (and range up to disastrous in a small number of cases, where, for example, a fistula results). But give most men a choice between wearing depends and being dead and the choice isn’t that hard. The problem is in not knowing if death really was the alternative. Someday we may be able to know with relative certainty; but not today.
@WereBear:
The problem with determining overtreatment of breast and prostate cancers is that we can’t tell beforehand which cases don’t need to be treated.
As I wrote above, a radiation oncologist who specializes in treating prostate cancer, told me that he felt sure we overtreat prostate cancer, but the problem is in knowing which is which — those cancers we should treat and those who need to be watched. Absent the ability to tell the difference, many, if not most men will opt for aggressive treatment, since they won’t get a second chance.
Mnemosyne
@Wag:
Okay, that makes more sense. By the current guidelines, even as someone with a family history he probably doesn’t need to get his first PSA until he’s at least 55, but your first post made it sound like you didn’t recommend it for anyone, even people with a family history.
I think that’s the thing that’s missing from Richard’s matrix: family history. Someone who knows that their grandfather/grandmother/father/mother/sibling had a specific cancer probably needs to be screened earlier and treated a little more aggressively, if necessary, but people screech if you point that out. Yes, you have outliers (like, so far, my mother) who develop aggressive cancers at a young age but no one else in the family does, but that doesn’t seem to be common enough to demand that everyone get screened every year.
(I keep trying to tell my doctor that I don’t necessarily need a pap smear every year since they’ve always come back normal and I’ve been in a monogamous relationship for almost 15 years but, nope, gotta get it every damn year.)
Fair Economist
@Wag: Actually, looking at those studies, they’re all either hopelessly contaminated by PSA tests in the “control” group, or they’re too short to really test the benefits of PSA screening. The longest followup in the randomized trials was 9 years, which is not really long enough to detect the benefits of screening. Basically this is one or two rounds of screening, not the outcome of a lifelong screening process, which is IMO how it should be done.
Based on the relatively high cancer mortality among treated patients, when the PSA caught a cancer it was usually metastatic. I suspect that the overwhelming majority of those “catches” were in the first screening. So the problem is that they start screening too late.
There is certainly a problem with overtreatment of suspected prostate cancer cases. Based on those studies, I’d say we need *more* screening but less treatment. One specific idea I have is that the PSA test should be described as a “prostatic irritation test” rather than a “prostate cancer test”. That might help with the panic many men have at an elevated PSA. It’s more accurate, as well.
Mnemosyne
@TriassicSands:
I have a metastasization question that’s been bugging my family for a while now — hopefully someone can jump in if they know the answer. My father-in-law was diagnosed and treated for prostate cancer, which was successfully treated with radiation (at least, as far as we knew at the time). A few years later, he developed a glioblastoma multiforme brain tumor. The neurosurgeon who biopsied the tumor said it was a result of the prostate cancer metastasizing, but the oncologist disagreed. Any clue who might have been right?
azlib
@TriassicSands:
I agree with your take on this issue. Your post reflects my own experience with the disease. I will also say that you are never “cured” even with surgery which looks clean. You are always in “surveillance” mode. There is always a small, but positive probability that microscopic tumors escaped the prostate which are undetectable until they create problems. In my case that probability is very low, since my surgery had “clean” edges and no cancer in the seminal ducts (which also get removed in surgery).
I will continue to have a PSA test yearly after my two year surgery anniversary and it will hopefully remain “undetectable”.
Wag
@Mnemosyne:
If the tumor was a glioblastoma, then the tumor was a second primary cancer, not a metastasis from the prostate cancer. By looking at the tumor under the microscope it is sole to differentiate a glio from a glandular tumor like prostate. The two look nothing alike. Reading the pathology report will settle the issue.
Wag
@Mnemosyne:
Cervical cancer is a sexually transmitted disease caused bye HPV If your Pap is normal and you test negative for HPV, then you need your next Pap in 5 years, not annually.
Fair Economist
Wow, the biopsy scores are done on tissue morphology? That’s pretty primitive, especially now that we now know cancer is usually preceded by significant chromosomal and genetic changes. And sure enough, here’s a paper showing a huge additional predictive value from screening biopsies for chromosomal 8 changes link Basically, on “iffy” biopsies of Gleason 6, the absence of chromosomal 8 changes largely excluded the possibility of 4+3 grade cancer elsewhere in the prostate.
Mnemosyne
@Wag:
After I posted that, I remembered that I have a confounding factor: my mother was given DES while she was pregnant with me. So I probably am stuck with annual pap smears regardless of my sexual history.
jl
@Wag:
“insensitive” I think you meant non-specific.
@Fair Economist:
I don’t think the problem is that follow-up is not long enough. Everyone dies of something sooner or later, so the longer you wait, the less meaningful survival rate statistics are, mostly due to contamination with competing risks of death. Statistically, trying to untangle survival rate for a specific cause of death due to an intervention is very difficult as the probability of death to a competing risk rises. And for all of us, that risk rises towards one.
Standard survival rates are based on five year follow-up.
A standard survival rates statistic will be greatly influenced by stage at detection, and these are very difficult to control for between populations. The very high survival rates form a few cancers in the U.S., and prostate cancer is an example, are almost certainly due to detection of cancers with low probability of casing harm at much earlier stages than in other countries.
Patient preferences for treatment also influence survival rates. I’ve read that the relatively low survival rate for breast cancer in the U.K. compared to the U.S. and other high income countries that prevailed in the 90s and early 00s was deemed to be jointly caused by inadequate screening programs, and deference of U.K. docs to patient preference for lumpectomies versus radical mastectomy. (Edit: surprisingly to some, the NIH in UK was willing to give more conservative treatments to patients who wanted them much earlier than in U.S.)
Survival rates are very tricky things to use to judge the merits of how a health care system is detecting and treating a disease. They are more appropriate for evaluation of prognosis for an individual or a very carefully defined sub-population of patients.
Better to use population mortality rates, adjusted for population risks, to judge the relative performance of different system’s performance. A commenter provided a link to a very good video explaining why, but I forget which thread. It was a couple of weeks ago. (Edit: maybe if that commenter drops by, could repost it)
Wag
@Mnemosyne:
Yes, you are. Bummer.
Wag
@jl:
Nicely said.
mellowjohn
@TriassicSands:
as mentiioned in my comment at #29, my Gleason score was a 4+3.
also too, as part of my therapy, i was given 2 injections of Lupron, spaced 3 months apart. i had the full array of side effects: fatigue, hot flashes, night sweats, and wild mood swings.
my wife suggested that every male med school grad should go thru Lupron shots to help them have more sympathy for women going thru menopause.
Fair Economist
The problem with the followup times is that the period between metastatic spread of the cancer (when it’s too late to cure) and death (before which it’s too early to measure) is typically over 5 years. So for the vast majority of patients in the study, either it started too late to screen them in time or it started too early for them to have died of the cancers it caught. You need a study substantially longer than the time to go from detection to possible death or it’s not useful.
Richard Mayhew
@dnfree: The one time I try to use a cute song lyrics, everyone has to ruin my buzz with reality :)
Wag
@Richard Mayhew:
Boston rocks!!!!!
jl
@Fair Economist: But, as I said, as the follow-up time grows longer, the harder it is to get estimates of the proportion surviving over the time horizon that is due to specific interventions that are due to the disease of interest that is independent of other causes of death, unless a lot of factors like age, treatment, stage at diagnosis, comorbidities are independent of the disease. But usually they are very dependent.
So, big trade off between time horizon chosen for analysis, and reliability and consistency of the estimate.
Someguy
@Wag: With each prostate biopsy there a small but real chance of infection and bleeding. Also, keep in mind the prevalence of clinically meaningless cancer. By age fifty, 50% of men will have a small focus of clinically meaningless prostrate cancer. At age sixty, 60% will have cancer. Each biopsy increases the risk of finding one of those clinically meaningless cancers and prompting clinically harmful and unnecessary treatment.
So, odds are, we shouldn’t bother screening for it, because most men won’t die from prostate cancer, and it could be dangerous to treat it. Got it. Say, it’s easy to bend the cost curve.
Talentless Hack
I had a PSA, and it came back with a 2. The doc who ordered it wants me to take another one. She has this catchphrase she keeps repeating every time I see her – I don’t treat statistics; I treat patients. Sounds like an advertising jingle, doesn’t it. Well, I still haven’t had my second, follow-up PSA, and I’m not going to. From what I read on the paranoia machine, the threshhold for being even the slightest bit concerned is 4.
My guess is, I’ve been diagnosed with having a good insurance plan, and they intend to milk it for all it’s worth. So if I get that second, completely unnecessary (IMO) PSA, and it also comes back a 2, then what? She orders a biopsy?
I go see my regular doc in a week, and if he doesn’t mention it, I’m not either.
mclaren
…And so once again the ultrawealthy one-percenter Richard Mayhew vomits out an elaborate article based on ginning up wildly overpriced PSA tests of such dubious value that the medical profession itself recommends people not take routine PSA tests. And once again Richard Mayhew, our resident $800,000 man, talks about insanely expensive “options” like prostate biopsies.
Why not just urge the general public to buy gold ingots and throw them at doctors, Richard?
Why not simply explain the alleged “health benefits” of giving American doctors a ticker-tape parade using hundred-dollar bills instead of ticker tape?
Between the greedy inept American doctors who charge absurd amounts of money for worthless garbage tests like the PSA, and greedy corrupt insurance CEOs like the superwealthy one-percenter Richard Mayhew promoting overpriced diagnostic procedures of extremely dubious value, looks like it’s the American public that’s getting a colonoscopy…from the greed-crazed medical profession Richard Mayhew represents.
azlib
@Talentless Hack:
Find another physician. The threshold is 4. My PSA slowly increased over time until it went over the threshold and then I had a biopsy. It is pretty normal to have an increase in PSA as you age.